ARCHIVE
Dopamine has been making headlines these days. Check out some of the latest articles on this feel-good neurochemical: “Can dopamine décor make your home a happier place to be?” (Cosmopolitan) “‘Dopamine dressing’ is our new post-pandemic salve” (Mic) “Break the cycle of addiction with these strategies to keep dopamine in check” (NPR) Why is dopamine top of mind? A growing number of people are aware of dopamine’s influence on pleasure, but this unique neurotransmitter is involved in so much more. For example, it helps with focus and staying on task. Dopamine supports the brain’s ability to recall life’s significant moments, whether good or bad. Dopamine can be likened to a “chemical of more.” You always want more dopamine since it is the principal neurotransmitter that makes you feel good. Let’s take a deeper dive into this fascinating neurochemical and the myriad roles dopamine plays in our well-being. Why is dopamine top of mind? A growing number of people are aware of dopamine’s influence on pleasure, but this unique neurotransmitter is involved in so much more.WHAT IS DOPAMINE?
The dopamine system is complex. Dopamine-producing cells are found in the ventral tegmental area in the brainstem and the substantia nigra as well as other brain structures. Dopamine is the neurotransmitter of wanting, especially wanting more. It is the most critical player in the brain’s reward system, thus we have a natural proclivity for increasing dopamine. It is involved with anticipation, possibility, love, and seeking success to maximize future resources. Expecting a reward (food, sex, money, shopping) triggers dopamine release or when you get an unexpected happy surprise. Dopamine activates motivation (going toward a reward), memory, mood, attention, and other important features of mental health. Conversely, low dopamine levels can have an adverse effect. (Some of the symptoms of low dopamine are described below) Think of dopamine as a salesman that drives you to pursue a better life. But like many salesmen, it can also lie to you and promise you pleasure when, in fact, pain will result. For example, think of cocaine addiction or other addictive behavior, unhealthy habits, or having affairs. Even the anticipation of these harmful activities produce dopamine. Dopamine also helps to regulate motor control, which is why you jump when you get excited, such as when your team wins the World Series, or when your child hits a home run in Little League. There are 2 main brain dopamine systems in the reward pathway that relate to happiness:- The dopamine reward center in the front half of the nucleus accumbens of the basal ganglia (involved with seeking pleasure and addiction). Think of the dopamine reward system involved with wanting and desire.
- The dopamine control center that enhances the activity of the prefrontal cortex/orbitofrontal cortex and helps you think before you act and stop unhelpful behaviors. The dopamine control center is involved with forward-thinking, judgment, planning, impulse control, and long-term happiness.
CAN DOPAMINE IMBALANCES CAUSE PROBLEMS?
For happiness and a healthy sense of drive, dopamine plays a critical role, but it needs to be balanced. Too much or too little of it causes problems. For example, too much dopamine has been associated with mental health problems like agitation, obsession or compulsions, psychosis, and violence. Of the more than 100 murderers who have had brain SPECT imaging done at Amen Clinics, nearly half of them committed their crimes when they were on methamphetamines, which raises the brain’s dopamine level to an abnormally high amount. Low dopamine levels in the brain’s reward center can cause adversely affect brain function and lead to apathy, fatigue, boredom, low motivation, impulsivity, sugar cravings, and thrill-seeking and conflict-seeking behavior. It’s also associated with some neurological and medical conditions such as Parkinson’s disease. Dopamine deficiency is also thought to be related to attention deficit hyperactivity disorder (ADD/ADHD), which is associated with short attention span, distractibility, disorganization, procrastination, and impulse control issues. Many people with attention deficit hyperactivity disorder play the game of “Let’s have a problem” in an unconscious attempt to stimulate low dopamine levels. Needless to say, the brain’s dopamine balance is essential for good mental health.9 WAYS TO BALANCE DOPAMINE LEVELS NATURALLY
Knowing how to balance dopamine is fundamental to happiness and physical health. Here are 9 natural ways to help ensure your brain is making enough dopamine.1. Consume foods high in tyrosine.
One of the amino acids and important building block for dopamine, tyrosine can be found in almonds, bananas, avocados, eggs, beans, fish, chicken, and dark chocolate. These tasty foods increase dopamine levels naturally.2. Try a balanced diet that’s higher in protein-rich foods and lower in carbohydrates.
In animal studies, ketogenic diets have been shown to increase dopamine availability in the brain. Eating highly processed and sugary foods leads to cravings and overeating, which can reduce the sensitivity of dopamine receptors in the pleasure centers in the prefrontal cortex and lead to weight gain. Being overweight can impair dopamine pathways and neurotransmitter function. You can boost dopamine levels by making some simple changes to your diet.3. Make physical exercise a habit.
Physical activity increases levels of dopamine, while slowing down brain cell aging. Exercise has also been associated with improved mood and a better overall outlook on life. It’s the perfect way to get a natural dopamine hit.4. Say “om.”
Hundreds of research studies have demonstrated the overall health benefits of prayer and meditation (or focusing your mind). One found that dopamine release increased 65% following a single hour of meditation.5. Get a rubdown.
Exciting research has demonstrated that massage therapy increases dopamine levels by about 30% while decreasing the stress hormone cortisol.6. Get adequate sleep.
To ensure that your brain increases dopamine naturally, make sure you get enough sleep. Lack of sleep has been shown to reduce concentrations of neurotransmitters, including dopamine, and their receptors.7. Listen to calming music.
It’s no surprise that listening to calming music can increase pleasurable feelings, improve mood, reduce stress, and help with focus and concentration. Research has demonstrated that much of this occurs because of an increase in dopamine levels.8. Go outside.
Sunlight exposure increases dopamine in the brain, according to research, and is another helpful way to boost lower dopamine levels9. Take nutritional supplements.
The herbals ashwagandha, rhodiola, and panax ginseng have been found to increase dopamine levels, promoting improved focus and increased energy while enhancing endurance and stamina. Other supplements that increase dopamine include curcumins, l-theanine, and L-tyrosine, which promote alertness, attention, and focus. Depression, violence, obsessions and compulsions, and other mental health issues can’t wait. At Amen Clinics, we’re here for you. We offer in-clinic brain scanning and appointments, as well as mental telehealth, clinical evaluations, and therapy for adults, teens, children, and couples. Find out more by speaking to a specialist today at 888-288-9834 or visit our contact page hereAutism, or autism spectrum disorder (ASD), is diagnosed in 1 in 54 children, according to the CDC. The condition is associated with an array of challenges, including abnormal social skills, developmental delays, communication problems, and behavioral issues.
According to research, over 70% of children with autism spectrum disorder have at least one co-existing physical or mental health condition, and 40% have two or more of them. Among children with autism:
-
30-61% have ADHD
-
11-40% have anxiety disorders
-
7% have depression
-
Over 50% have chronic sleep problems
-
32% are overweight (2 to 5 year-olds)
-
16% are obese (2 to 5 year-olds)
In addition, kids with autism are 8 times more likely to have gastrointestinal issues compared to those who don’t have the condition. It is not unusual for them to have food allergies or food sensitivities.
Among adults with ASD, 26% have depression and 4-35% have schizophrenia (compared to 1.1% of the general population).
All of these challenges and symptoms can range from mild to severe. And a child’s diet (or an adult’s) can have an impact on severity. So, if you’re wondering what foods to avoid with autism spectrum disorders, you’ve come to the right place!
AUTISM AND THE BRAIN
Having seen more than 1,000 patients with autism spectrum disorder (ASD) at Amen Clinics, one of the first lessons we learned is that the ASD condition is not caused by one specific thing in the brain; there are actually 8-10 different factors that influence abnormal brain function.
We see ASD brains through SPECT imaging that are wildly overactive – often due to an inflammatory process. For others, we see brains with dramatic under-activity, which may be due to a toxin or some type of insult or injury to the brain.
This is one of the reasons why it is so important to look at brain function when coming up with a treatment plan for ASD. Throwing medication-tipped darts in the dark can hurt people.
However, there is one thing that all people with ASD should do regardless of whether their brains are overactive or under-active…eliminate anything that can hurt their brain health. This often means making dietary changes and eliminating specific foods.
THE FOOD YOU EAT MATTERS
It is important to realize that the food you eat is either medicine or it is poison. It is either helping your brain, body, and mind or hurting them. In other words, eating habits impact health, so it is important to avoid foods that can worsen symptoms.
We understand that children and adults with autism spectrum disorder are often known for picky eating and have certain food aversions or food preferences. However, dietary considerations are important in helping to manage autism spectrum disorder.
Here are the top 5 foods to avoid because they can adversely affect an otherwise healthy diet and make ASD and co-occurring condition symptoms worse.
1. DAIRY
When casein (one of the proteins in milk and dairy products) mixes with stomach acid, it produces something called an exorphin.
Exorphins bind to the opioid receptor sites and can result in a variety of troubles, including brain fog, spaciness, inability to concentrate, and a numbness to pain, just to name a few. A casein-free diet can reduce symptoms such as those.
Dairy is also problematic because it is considered one of the most pro-inflammatory foods in the Standard American Diet. According to a growing body of evidence, including a 2018 study in Pharmaceuticals, research suggests that inflammation is strongly associated with autism and is also commonly linked to immune system dysfunction.
This study shows that neuro-inflammation and neuro-immune abnormalities are key factors in the development and maintenance of ASD.
Avoiding anything that promotes inflammation is critical for anyone with autism spectrum disorder.
Gastrointestinal symptoms are fairly common with this condition, and in our experience, when people with ASD avoided dairy products, they began talking more, their hyperactivity was reduced, and bowel problems were resolved.
2. GLUTEN
Research shows that gluten—a mixture of proteins found in grains such as wheat, barley, and rye—can increase systemic inflammation when ingested. In fact, your body can create antibodies to gluten which can fire up, or inflame, your brain.
Gluten also decreases good bacteria in the gastrointestinal system, which is associated with an increased likelihood of feeling anxious, stressed, or depressed. The gut-brain connection in autism is real, according to findings in a 2019 study.
Gluten seems to particularly negatively affect the functioning of the cerebellum. Located at the back bottom of the brain, the cerebellum is involved with motor and thought coordination and is essential for processing complex information.
Through the brain-imaging work at Amen Clinics, we have discovered that those with autism spectrum disorder already often have decreased functioning of their cerebellum. Consuming gluten can make it much worse.
Although the research is mixed, many parents with autistic children report seeing improvements in symptoms after they put them on a gluten-free diet.
3. CORN
In the U.S., per capita consumption of corn products has risen from 28.4 pounds per year in 2000 to a whopping 35.2 pounds per year in 2019, according to Statista.
Since 1972, corn has been the top pesticide-using crop in the nation, based on findings from the USDA. A growing body of research, including a 2013 study in the journal Entropy, suggests a potential link between exposure to the herbicide glyphosate and the risk of autism.
Additionally, corn has the most unhealthy fatty-acid profile (high in omega-6 fatty acids that promote inflammation, compared to omega-3 fatty acids that are anti-inflammatory) of any of the whole grains. Yes, you read that right, grain. Corn is not a vegetable.
Another reason corn is one of the worst foods is that it has been found to be a breeding ground for fungi. In fact, a 2015 study identified 46 fungal isolates derived from maize grains.
There is simply nothing truly beneficial and many potentially harmful things that can come from eating corn. This grain is not necessary for getting the essential nutrients you need.
4. SUGARY SNACKS/REFINED CARBS
Not only are sugary foods pro-inflammatory, but it also increases erratic brain cell firing, and it is very addictive.
In addition, research appearing in Frontiers in Endocrinology found that people with ASD, like those with type 2 diabetes, have impaired glucose tolerance and excessive levels of insulin (a condition known as hyperinsulinemia). Because of this, consuming sugar may magnify improper insulin signaling.
Research in Plos One also shows that children on the autism spectrum who also suffer from gastrointestinal distress have poor metabolism of sugars. In these children, scientists found deficiencies in the levels of enzymes and transporters involved in the digestion of sugars.
Avoiding sugar and refined carbohydrates, including sugary snacks and cereals, and increasing consumption of lean proteins can dramatically improve concentration and judgment, and decrease impulsiveness.
5. ARTIFICIAL INGREDIENTS
A 2019 study suggests that the spike in autism may be connected to the preservatives found in processed foods. Other research points to a possible link between autism symptoms and artificial ingredients in our food supply.
Avoid all artificial additives, preservatives, dyes and artificial colors, artificial flavorings, and artificial sweeteners. Although these things are not really “foods”, they are found in so many food products that we wanted to list them here.
These substances can make autistic symptoms worse and are definitely unnecessary for proper nutrition.
If you or a loved one has ASD, paying close attention to the foods being consumed is particularly important.
For our patients with autism, we often recommend an elimination diet. This involves eliminating gluten, dairy, sugar, corn, soy, and other categories of potentially allergenic foods for one month.
Then add these back one at a time and be alert for reactions to them, which would indicate that your child’s nutrition plan should exclude that food.
Along with diet, other areas should also be investigated to uncover and address the challenges of ASD.
Autism and other mental health issues can’t wait. At Amen Clinics, we’re here for you. We offer in-clinic brain scanning and appointments, as well as mental telehealth, clinical evaluations, and therapy for adults, teens, children, and couples. Find out more by speaking to a specialist today at 888-288-9834 or visit our contact page here.
True crime is one of the most popular genres these days, and Americans can’t seem to get enough of these tales of murder, deception, and scandal. The Jinx, I’ll Be Gone in the Dark, Dirty John—these are just some of the true crime stories that have captured our collective attention. The one burning question that all these books, documentaries, and TV series ask is why? Why did they do it? The storytellers often point to many external factors—love, money, revenge—as the motives behind why people kill, cheat, and lie. But there’s one thing they’re missing—the brain. At the foundation of all these heinous acts is brain dysfunction. Yet, nobody is talking about it. In this blog, you’ll discover how the brain is involved in literally every criminal act, every scandal, and every shocking case of deceit. More importantly, you’ll learn how improving brain health is the key to decreasing criminal activity. The one burning question that all true crime books, documentaries, and TV series ask is why? Why did they do it? There’s one thing they’re missing—the brain. At the foundation of all these heinous acts is brain dysfunction.TRUE CRIME IN THE BRAIN
For over 30 years, Amen Clinics has been performing brain scans on patients using an advanced technology called single photon emission computed tomography (SPECT). SPECT measures blood flow and activity in the brain. SPECT scans reveal areas of the brain with healthy activity, too much activity, and too little activity. Amen Clinics has built the world’s largest database of functional brain scans related to behavior with over 300,000 SPECT scans. Based on these brain scans, it’s clear that when parts of the brain are overactive or underactive, it’s associated with emotional, cognitive, and behavioral problems. In general, the brains of murderers, cheaters, and thieves don’t look healthy. Here are 5 ways the brain impacts criminal behavior.-
Aggression is related to 3 brain activity patterns.
- Impulsive Aggressive Type: This type is associated with reduced blood flow in the frontal lobes (hypofrontality). Research has linked this type to antisocial personality disorder. Individuals with low blood flow in the prefrontal cortex (PFC) often struggle to control aggressive impulses, increasing the likelihood of committing violent acts.
- Compulsive Aggressive Type: This type is found in people with too much activity in the frontal lobes (hyperfrontality). These individuals tend to explode due to cognitive inflexibility or getting stuck on negative thoughts.
- Temporal Lobe Abnormalities: This type involves abnormal blood flow levels in the temporal lobes and/or frontal lobes. In an analysis of SPECT and MRI scans involving 21 violent offenders convicted of impulsive crimes, experts found that 16 of the criminals had varying levels of reduced blood flow in these brain regions. The perpetrators’ MRI scans, however, showed no anatomical problems or other abnormalities.
-
Murderers may have low blood flow in the brain.
- Left medial temporal lobe
- Inferior orbital prefrontal cortex
Healthy Surface SPECT Scan
 Full, even, symmetrical activity.
Full, even, symmetrical activity.
Kip Kinkel’s Surface SPECT Scan
 Several areas of low blood flow (the areas that look like holes indicate low blood flow)
Kinkel’s brain scans also showed overall low activity throughout the brain.
Several areas of low blood flow (the areas that look like holes indicate low blood flow)
Kinkel’s brain scans also showed overall low activity throughout the brain.
Healthy Active SPECT Scan
 A healthy “active” scan shows the most active parts of the brain with blue representing the average activity and red (or sometimes red and white) representing the most active parts of the brain. In the healthy brain, the most active area is in the cerebellum, at the back/bottom part of the brain.
A healthy “active” scan shows the most active parts of the brain with blue representing the average activity and red (or sometimes red and white) representing the most active parts of the brain. In the healthy brain, the most active area is in the cerebellum, at the back/bottom part of the brain.
Kip Kinkel’s Active SPECT Scan
 Severe underactivity throughout the brain
Severe underactivity throughout the brain
-
Murderers may have overactive brains.
- Prefrontal cortex—associated with forethought, judgment, and empathy
- Anterior cingulate gyrus (ACG)—the brain’s gear shifter, intended to help people go from one thought to another or one action to another
-
Traumatic brain injuries (TBIs) are linked to criminal behavior.
-
Hidden dementia can lead to criminal behavior.
-
In some cases, standard mental health treatments can worsen symptoms.
CAN THE CRIMINAL BRAIN BE REHABILITATED?
The brain and mental health professionals at Amen Clinics have spent more than three decades helping people enhance their brain health and improve their life. This goes for people with a criminal history too. In general, better brain function leads to better decision making, better judgment, and better behavior. Focusing on increasing brain health at the earliest signs of trouble may be a way to avoid the shocking behavior that leads to all those true crime stories. Aggression, violence, and other mental health issues can’t wait. At Amen Clinics, we’re here for you. We offer in-clinic brain scanning and appointments, as well as mental telehealth, clinical evaluations, and therapy for adults, teens, children, and couples. Find out more by speaking to a specialist today at 888-288-9834 or visit our contact page here.Content updated from previous publish date.
Skittles—sweet treats or toxic chemicals? A 2023 bill passed in California aims to ban several ingredients found in many candies and snack foods. The four ingredients that have been targeted by the state’s lawmakers are propylparaben, potassium bromate, brominated vegetable oil, and Red Dye 3.
These are toxic chemicals that can have adverse affects on physical and mental health and cause behavioral changes.
The bill originally included another ingredient called titanium dioxide, which is found in Skittles. This led people to believe the popular candy would get yanked from store shelves, which is how the bill got nicknamed the “Skittles ban.”
But Skittles doesn’t have any of the ingredients named in the ban, so they will still be available for sale.
Just because they are on store shelves, however, doesn’t mean they’re good for your brain or mental health. In fact, Skittles and other foods and drinks that are red in color can have harmful effects. In part, this is because they contain another commonly used artificial food coloring called Red Dye 40.
The use of Red Dye 40 is concerning because it has been linked to adverse effects, such as a host of physical and mental health issues, including ADD/ADHD, allergies, immune disorders, mind storms (which are issues with the brain’s wiring or electrical activity), and even inflammatory bowel diseases.
Red Dye 40 has been linked to a host of physical and mental health issues, including ADD/ADHD, allergies, immune disorders, mind-storms, and even inflammatory bowel diseases.CLICK TO TWEET
THE TRUTH ABOUT RED DYE 40
Horrifyingly, the food industry dumps 15 million pounds of synthetic food dyes into what we eat every year—over 40% of which is Red Dye 40, a petroleum-based substance. Red Dye 40 is the number-one food dye used in the United States, found in most unnaturally red foods. According to a 2010 article by the Center for Science in the Public Interest (CSPI), consumption of such dyes has increased five-fold since 1955.
There are 9 artificial dyes used in our food supply that are certified by the Food and Drug Administration (FDA).
Even though there are safe and natural alternatives available, artificial food dyes are a cheap way for manufacturers to make processed foods brighter and more appealing when you see it on a shelf in the grocery store. Manufacturers also choose artificial coloring because it provides more uniform colors compared to natural food coloring.
Artificial dyes are also used to help hide the fact that many processed foods don’t contain much (or any) of the nutrients or foods they claim to have. For example, without Red Dye 40, the chocolate instant pudding would actually look green (because there’s VERY little real chocolate in it).
Although Red Dye 40 has been approved by the FDA for use in food products and must be listed as an ingredient on labels, it has been banned at one time or another throughout Australia and other countries, including most of Europe, due to health concerns.
SURPRISING FOOD ITEMS CONTAINING RED DYE 40
Not all of the foods with Red Dye 40 are red. You will also find it in brown, blue, green, orange, and even white food products, too. Take pickles for example. A combination of artificial dyes, including Red Dye 40, is used to give some pickles a more pronounced yellow-green color.
You can find Red Dye 40 in a wide range of foods and beverages, including:
-
Candy
-
Condiments
-
Snack foods
-
Baked goods
-
Beverages, including energy drinks
-
Salad dressings
-
Dairy products
-
Frozen desserts
-
Breakfast cereals
-
Fruit bars
-
Sauces
Food items aren’t the only place you’ll find this artificial dye. Many personal care products, such as toothpaste and mouthwash, can be artificially dyed. Even more disconcerting, some prescription medications may be tinted with the stuff.
THE CONNECTION BETWEEN RED DYE 40 AND ADD/ADHD
Multiple studies published in journals such as Pediatrics, The Lancet, and Journal of Pediatrics demonstrate that some children with ADD/ADHD may be adversely affected by artificial food colors. Other research indicates that artificial coloring and flavors, as well as the preservative sodium benzoate, can make some non-ADD/ADHD kids hyperactive.
Some children who have been diagnosed with ADD/ADHD and are taking medications for the condition make such an improvement after eliminating Red Dye 40 from their diet that they are able to stop taking their prescription drugs.
Many parents who notice increased hyperactivity in their children after a sweet snack mistakenly blame a “sugar rush” for the bad behavior. But often, it’s the artificial food coloring that’s the real culprit.
Additionally, both adults and children have reported upset stomach, migraines, jitteriness, nervousness, and inability to concentrate after a high intake of Red Dye 40. The CSPI released a report that says artificial food dyes pose a “rainbow of risks,” including everything from allergies to cancer.
DOES RED DYE 40 TRIGGER ABNORMAL BRAIN ACTIVITY?
Artificial dyes may also trigger “mind-storms,” which are issues with the brain’s wiring or electrical activity. Your brain is the world’s most powerful hybrid electrochemical engine. It uses electricity and neurotransmitters to help you think, feel, and act.
Abnormal electrical activity can not only change the activity of the brain, but it can also change your mind and cause mind storms that can be associated with temper outbursts, depression, suicidal thoughts, panic attacks, distractibility, and confusion.
CAN RED DYE 40 LEAD TO INFLAMMATORY BOWEL DISEASES?
The downsides of Red Dye 40 also include problems with inflammatory bowel diseases (IBD). A 2022 study on mice in Nature Communications found that frequent consumption of artificially colored red foods like Lifesavers, Jell-O, and Gatorade increases the chances of developing an IBD, such as Crohn’s disease or ulcerative colitis.
The findings suggest that long-term exposure to the dye in quantities commonly consumed in food products damages gut health and raises the risk of inflammation. According to the study, artificial food coloring impairs the gut’s lining, which typically acts as a barrier, allowing bacteria to permeate the gut and disrupting the microbiome.
“What we have found is striking and alarming, as this common synthetic food dye is a possible dietary trigger for IBDs,” said study author Waliul Khan in a press release. “This research is a significant advance in alerting the public on the potential harms of food dyes that we consume daily.”
RED DYE 40 AND THE BRAIN
The brain imaging work at Amen Clinics demonstrates that Red Dye 40 can dramatically affect brain function. Consider the case of Robert, a 15-year-old who underwent brain SPECT imaging at Amen Clinics. SPECT is a functional brain imaging tool that measures blood flow and activity in the brain.
His parents noticed that whenever Robert ate or drank something bright red, his behavior became aggressive and hostile. He would easily cry and storm off in a huff or throw things. They brought him to Amen Clinics to confirm their suspicions that he was reacting to these food additives.
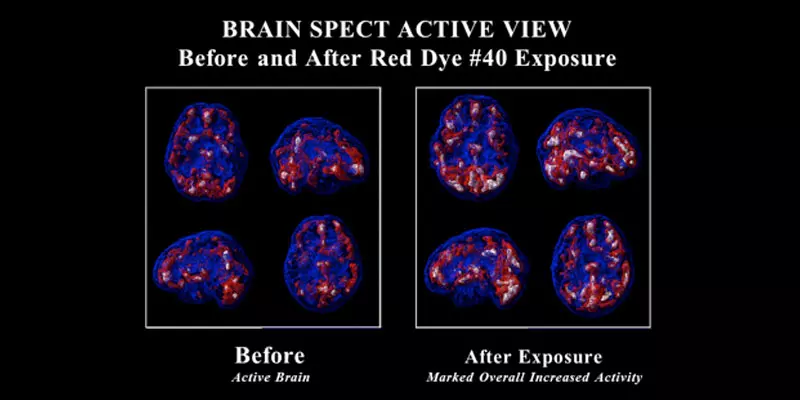
As can be seen on this teen’s SPECT scan, his brain showed remarkable overall increased activity with exposure to Red Dye 40. In the images, blue equals average activity, red equals the top 15% of brain activity, and white equals the top 8% of brain activity.
After removing Red Dye 40 from his diet, Robert’s behavior improved dramatically. His mother strongly believes that their experience is not a unique one and that Red Dye 40 should be completely banned from our food supply.
HOW TO SPOT FOOD DYES ON NUTRITION LABELS
A new field called nutritional psychiatry shows how important food is for mental health, emotional well-being, cognitive function, and behavioral stability. Knowing that you are what you eat, no discussion about changing your diet can miss the importance of eliminating this substance!
To rid this dye from your family’s diet, you need to learn to scour nutrition labels. Red Dye 40 goes by many names. Look for any of these ingredients on labels:
-
Allura Red
-
Allura Red AC
-
C.I. 16035
-
C.I. Food Red 17
-
FD&C Red No. 40
-
Red 40
-
Red No. 40
Be aware that even though food manufacturers are required to list the dye on nutrition labels, they don’t have to specify how much is included. Your best strategy is to steer clear.
HOW TO KNOW IF FOOD DYES ARE AFFECTING YOU
An elimination diet can help you determine if artificial food dyes may be contributing to bothersome symptoms. For one month, cut out sugar, gluten, dairy, corn, and soy, as well as artificial dyes, additives, and preservatives to see if you feel better. Then add these substances back one at a time and be alert for reactions to them, which would indicate that you should permanently avoid that food.
ADD/ADHD, behavioral problems, and other mental health issues can’t wait. At Amen Clinics, we’re here for you. We offer in-clinic brain scanning and appointments, as well as mental telehealth, clinical evaluations, and therapy for adults, teens, children, and couples. Find out more by speaking to a specialist today at 888-288-9834 or visit our contact page here.
Do you come home from work or have the day off and still feel utterly drained with no energy to do anything? You may be wondering if it’s just burnout from a demanding job or something more serious like clinical depression. In many cases, it can be difficult to know which one you’re dealing with. Oftentimes, terms like burnout and depression are used interchangeably, but these issues are not the same. And they require very different treatment plans. Terms like burnout and depression are used interchangeably, but these issues are not the same. And they require very different treatment plans. Understanding the nuances between them can be crucial for obtaining proper help. According to the National Institute of Mental Health, 8.3% of all U.S. adults have experienced a depressive episode. Meanwhile, a 2022 survey shows that 42% of the global workforce report burnout. How can you tell which one you have and how to overcome it? In this post, we’ll explore the differences, symptoms, and solutions associated with both burnout and major depressive disorder to help you identify and heal from whichever one you might be experiencing.
IS THERE A DIFFERENCE BETWEEN BURNOUT VS. DEPRESSION?
In short, yes. However, understanding which one you have may take a bit of digging. While burnout and depression are associated with similar symptoms, they stem from different causes that require distinct treatment. Here’s a breakdown of what causes burnout vs. depression, according to an international team of researchers:- Burnout is not considered a mental health disorder, rather it is typically related to chronic workplace stress. It can also be due to other issues like medical, interpersonal, or social stress.
- Depression is a mental health condition that affects your thoughts and behavior patterns. It is a brain-based disorder that can develop from a variety of factors including genetic predisposition, unhealthy brain function, neurochemical imbalances, and significant life events.
IDENTIFYING SYMPTOMS OF BURNOUT
If you’re feeling mentally, emotionally, and physically exhausted from dealing with repeated stress for too long, you may be experiencing burnout. Plus, it’s not just about work—parents, relationships, and caregiver burnout may leave you feeling endlessly tired, overwhelmed by responsibilities, or worried you’re not doing a good job. Burnout symptoms often include overwhelming fatigue, detachment from work, and a sense of ineffectiveness. These symptoms are more often directly related to prolonged workplace stress which can significantly impact job performance and satisfaction. Here are five symptoms of burnout to keep in check:- You may have chronic fatigue if you consistently feel physically and emotionally drained, even after a full night’s sleep.
- You may become detached and cynical if you’ve become increasingly negative, distant, and disengaged from work or personal responsibilities.
- You may see reduced performance if you’re struggling to concentrate, feeling less effective, and noticing decreased productivity.
- You may feel more irritable with mood swings if you’re experiencing heightened agitation, repeated frustration, and sudden mood changes.
- You may also have physical symptoms like headaches, dizziness, stomach or digestive issues, and other stress-related physical ailments.
RECOGNIZING SYMPTOMS OF DEPRESSION
Depression symptoms extend beyond interpersonal circumstances to permeate every aspect of your life. These symptoms include persistent sadness, loss of interest in previously enjoyed activities, changes in appetite or sleep patterns, and feelings of worthlessness or guilt. It’s important to know that you are not your thoughts. Here are five symptoms of depression to be mindful of when checking in on yourself:- You may feel persistent sadness if you have continuous feelings of unhappiness, hopelessness, or emptiness.
- You may feel worthless if you struggle with intense feelings of guilt, meaninglessness, or self-blame.
- You may feel a loss of interest with a diminished interest or pleasure in activities you once engaged in or enjoyed.
- You may have disrupted sleep like insomnia (inability to go to sleep) or hypersomnia (inability to stay awake), excessive sleeping, and grogginess.
- You may feel changes in appetite resulting in significant weight loss or gain with unhealthy nutritional choices for quick energy and inconsistent eating patterns.
SOLUTIONS TO HEAL BURNOUT SYMPTOMS
To overcome symptoms of burnout, you need to address the external factors that may be triggering an internal response. This may look like workplace changes, stress management strategies, and sometimes taking time off to recuperate. It’s not just about restoring your energy levels so you can get back to work. It’s about healing the mind-body connection, so you can prevent burnout symptoms in the future. Additional healing strategies include:- Create A Self-Care Routine: Make a habit of regular breaks, whole food nutrition, low-impact exercise, meditation, and relaxing daily hygiene.
- Seek Professional Support: Ask HR or a professional coach to address and find accommodations for certain work-related stressors.
- Make Lifestyle Changes: Find tangible solutions to your stressful work and home responsibilities to create a sustainable environment to heal symptoms.
SOLUTIONS TO HEAL DEPRESSION SYMPTOMS
For depressive symptoms, it’s about treating the root cause, which requires treatment from a mental health professional. A holistic brain-body approach is a powerful way to heal from clinical depression.- Engage In Therapy: Psychotherapy, such as cognitive behavioral therapy (CBT), can help you address negative or intrusive thought patterns, track behavior changes, and gain coping strategies.
- Take Nutrition Seriously: Consult your doctor to discuss your important health numbers and identify vitamin or mineral deficiencies and hormonal imbalances that can contribute to mood disorders.
- Build Brain-Healthy Habits: Regular exercise, a balanced diet, and adequate sleep cannot be overstated when it comes to supporting mental and brain health.
- Be Careful with Medications: Antidepressants are often prescribed as a common depression treatment, but research shows that two-thirds of people don’t respond fully to medication alone. A 2020 study found that combining CBT with prescribed medications significantly improved effectiveness compared to using medications alone.
- Consider Supplements: Nutraceuticals, such as saffron, can be effective mood enhancers. In fact, a double-blind, placebo-controlled clinical trial found saffron to be as effective as fluoxetine (Prozac) without the common side effects that come with antidepressants.
EFFECTIVE TREATMENT FOR BURNOUT AND DEPRESSION
Treatments for burnout and depression must be tailored to an individual’s specific condition. While there are overlapping strategies, recognizing the primary condition is crucial for effective treatment. The brain-imaging work at Amen Clinics can help identify types of depression by revealing abnormalities in brain function. Brain scan technology called single photon emission computed tomography (SPECT) helps pinpoint depression causes and provide a more accurate diagnosis. This leads to a better outcome in your depression treatment. According to a 2021 study, people experiencing burnout are prone to symptoms of depression, but that doesn’t result in a direct clinical depression diagnosis. Knowing the difference is key to finding the right treatment and support. Depression, burnout, and other mental health issues can’t wait. At Amen Clinics, we’re here for you. We offer in-clinic brain scanning and appointments, as well as mental telehealth, clinical evaluations, and therapy for adults, teens, children, and couples. Find out more by speaking to a specialist today at 888-288-9834 or visit our contact page here. By Rishi Sood, MD When you’re in a meeting, focusing on what your supervisor is saying or concentrating on a work project, there’s a specific part of your brain that’s especially active, helping you pay attention. This brain system is known as the dorsal attention network (DAN). The DAN plays a crucial role in how you focus your attention on various tasks throughout the day, from studying to playing sports. When this brain network is functioning optimally, it helps you concentrate. When the DAN is not working as well as it should, it can make it harder for you to stay focused. It can also make you more vulnerable to certain mental health disorders. When the dorsal attention network is functioning optimally, it helps you concentrate. When it’s not working as well as it should, it can make it harder for you to stay focused.WHAT IS THE DORSAL ATTENTION NETWORK?
The dorsal attention network is a group of brain areas located primarily in the top and front parts of the human brain. Research shows that brain regions involved in the DAN include:- Intraparietal sulcus
- Frontal eye fields
HOW DOES THE DORSAL ATTENTION NETWORK WORK?
Think of the DAN as your brain’s control panel for attention. When you need to concentrate, the DAN lights up, helping you zero in on what’s important at that moment. It controls what you pay attention to by increasing your brain’s sensitivity to certain stimuli, like a teacher’s voice, and reducing sensitivity to others, like the chatter from classmates. Experts refer to this as top-down attention, where your brain chooses what to focus on. Your brain intentionally directs your attention to something that matters to you based on your goals and expectations. This differs from bottom-up attention, where your brain shifts its focus due to unexpected external changes, such as a loud noise or a bird flying right in front of your face.THE DORSAL ATTENTION NETWORK AND MENTAL HEALTH
The way the dorsal attention network functions is vital for your ability to focus, but it also plays a significant role in your mental health. Here’s how:- Attention-Deficit/Hyperactivity Disorder (ADHD): In people with ADHD, also known as attention-deficit disorder (ADD), the DAN might not function as effectively. This can make it hard to stay focused on tasks, leading to difficulties in school and while doing homework.
- Anxiety disorders: When you’re anxious, the DAN might become overly reactive to non-threatening stimuli, making you feel overwhelmed by everyday situations. This can distract you from important tasks and increase feelings of stress.
- Depression: Those experiencing clinical depression may find that their DAN doesn’t activate as strongly as it should. This can lead to problems with concentration and maintaining attention on tasks or activities that used to be enjoyable.
- Schizophrenia: Emerging findings from a 2023 brain-imaging study indicate that activity in the dorsal attention network is different in people with schizophrenia. This distinct activity occurs during visual perception organization and may be related to the cognitive disorganization seen in this mental health disorder.
SUPPORTING THE DORSAL ATTENTION NETWORK FOR BETTER MENTAL HEALTH
Understanding the role of the dorsal attention network can help us find better ways to support our mental health. Here are some strategies that can strengthen this network:- Mindfulness and meditation: Engaging in mindfulness exercises or meditation can help train the DAN to be more effective. These practices teach you to focus your attention deliberately, which can improve how well the DAN functions.
- Regular exercise: Physical activities, especially those that require concentration like team sports or martial arts, can enhance the functioning of the DAN. Exercise increases blood flow to the brain, which helps keep your neural networks healthy.
- Adequate sleep: Sleep is essential for brain health. A good night’s sleep helps reset brain networks, including the dorsal attention network, making it more effective during the day.
- Balanced nutrition: Eating a diet rich in nutrients supports overall brain health, which is crucial for the proper functioning of the DAN. Eating foods that are high in omega-3 fatty acids, like fish and nuts, are particularly beneficial. You may also want to consider taking omega-3 nutritional supplements.
BUSTING DEPRESSION MYTHS
Learning more about depression and offering informed support to those affected will ensure you’re part of the solution. Here, we’ll examine some of the most important, and most often misunderstood, points to keep in mind—the top 5 things depressed people wish you knew.-
Depression is a legitimate mental health symptom.
-
Depression is NOT a single condition.
-
People with depression need your support.
-
Depression is not a weakness or character flaw.
-
Depression isn’t always debilitating.
SUPPORTING LOVED ONES WITH MAJOR DEPRESSIVE DISORDER
When someone is struggling with a mental health disorder, life can feel overwhelming—for them and for the people who love them. The good news is that we have more options than ever before to treat and manage depressive symptoms. And, when they’re given understanding, acknowledgment, validation, patience, and support, people with depression have a much better chance of success. If you or a loved one have depression, make sure you’re offering all of the above to help pave a smoother road to recovery. Depression and other mental health issues can’t wait. At Amen Clinics, we’re here for you. We offer in-clinic brain scanning and appointments, as well as mental telehealth, clinical evaluations, and therapy for adults, teens, children, and couples. Find out more by speaking to a specialist today at 888-288-9834 or visit our contact page here. Does your child rarely or never comply with your requests? Do they tend to avoid responsibilities and struggle to complete tasks that most kids would find agreeable? Do they procrastinate, shut down, or act out aggressively when you ask them to do something? If so, you might want to familiarize yourself with the symptoms of pathological demand avoidance (PDA). PDA is not an official diagnosis in the Diagnostic and Statistical Manual of Mental Disorders, Fifth Edition (DSM-5). Instead, it describes a set of behaviors and traits that can interfere with daily functioning. Pathological demand avoidance in kids also has its share of controversy and misunderstandings. Let’s look deeper at PDA’s characteristics, symptoms, and ways parents can cope. While most children will demonstrate defiant or avoidant behavior to some degree, PDA refers to persistent avoidance that interferes with daily life.WHAT IS PATHOLOGICAL DEMAND AVOIDANCE?
The term “pathological demand avoidance” was coined by British psychologist Elizabeth Newson as early as the 1980s. She made its official debut in the medical community through her 2003 review, “Pathological Demand Avoidance Syndrome: A Necessary Distinction within the Pervasive Developmental Disorders.” As the title suggests, Newson opined that PDA deserved to be recognized as its own entity rather than grouped into “pervasive developmental disorder not otherwise specified,” as it was in the then-current DSM-4. She also noted that PDA was found to be “significantly different on many counts from classic autism and Asperger’s syndrome.” Even today, PDA is closely linked with autism, since it’s most often seen in those with autism spectrum disorder (ASD). Experts have drawn connections between PDA and the challenges of sensory processing found in autism. But sensory challenges, as well as PDA, can be present without autism. Symptoms of PDA can also overlap with those of other mental health conditions, like attention-deficit/hyperactivity disorder (ADHD), complex post-traumatic stress disorder (CPTSD), or oppositional defiant disorder (ODD). And some children with PDA may have no diagnosed mental health disorders. Furthermore, when untangling the definition and diagnoses behind PDA, the National Autistic Society warns that very little research exists on this topic, “and the research that does exist is generally of a low quality. Because of this, many aspects of demand avoidance…are under-researched and often contested.” Even the name itself has been subject to controversy. Because of potential stigma surrounding the word “pathological,” alternative names have been suggested: persistent drive for autonomy, extreme demand avoidance, and rational demand avoidance.SIGNS OF PATHOLOGICAL DEMAND AVOIDANCE
Kids with pathological demand avoidance may be mistakenly labeled as troublemakers or defiant. They may appear so, since they’re likely to resist demands from others—and even their own demands. But their avoidance is not related to laziness, willfulness, or lack of intelligence. Rather, those with PDA tend to struggle with anxiety and rigid, inflexible thinking. While most children will demonstrate defiant or avoidant behavior to some degree, PDA refers to persistent avoidance that interferes with daily life. For example, while it might be normal for kids to occasionally refuse to do their homework or chores, a child with PDA can freeze up in the face of simple questions. Or they may deny their own bodily cues, such as avoiding hunger or thirst. The PDA Society notes that demands can take many forms, from direct requests to general expectations. Children with PDA (a spectrum disorder) have a range of responses to those demands. Avoidance tactics may be exhibited externally (overt avoidance), internally (feelings of anxiety), or both. Because these children can show avoidance in response to big and small demands, they may have trouble with tasks such as:- Completing schoolwork or chores
- Fulfilling their personal needs or desires
- Going to bed or waking up
- Making decisions, like choosing a meal from a menu
- Following instructions
- Answering questions
COPING WITH PATHOLOGICAL DEMAND AVOIDANCE SYMPTOMS
When children with PDA are misunderstood as “bad” or “lazy,” they’re likely to perform even worse in school and at home. While it’s important for parents to set consequences for behavior, tactics like enforcing overly strict punishments or ramping up the intensity of demands are likely to backfire. Instead, you and your child can learn how to work with their abilities and limitations rather than against them. When dealing with your child’s oppositional behavior, the Child Mind Institute recommends strategies such as:- Collaborating with your child on accomplishing tasks
- Avoiding arguing
- Using negotiation, compromise, flexibility, and creativity
- Finding and utilizing your child’s innate sources of motivation
- Helping them develop skills that will enable more independence
- Understanding that their compliance may look different than your expectations
- Behavior modifications
- Life skills training
- Nutritional supplements
- Sensory integration therapy
CREATING BETTER OUTCOMES FOR PDA
While pathological demand avoidance describes a set of behaviors that last throughout a lifetime, gentler approaches can make a world of difference in coping along the way. It’s crucial for parents and other authority figures to remain open-minded and nonjudgmental, rather than labeling these children as stubborn or defective. Learning and teaching them how to work with their differences will help prevent further hindrances to their performance. Using patience, understanding, and flexibility, you may change the course of their entire lives. Pathological demand avoidance and other mental health issues can’t wait. At Amen Clinics, we’re here for you. We offer in-clinic brain scanning and appointments, as well as mental telehealth, clinical evaluations, and therapy for adults, teens, children, and couples. Find out more by speaking to a specialist today at 888-288-9834 or visit our contact page here. Cults have always been a source of fascination. Groups like NXIVM, children of God, the Manson Family, David Koresh’s Branch Davidians, Heaven’s Gate, and Jim Jones’ Peoples Temple have spawned dozens of books, films, and cult documentaries. A recent Netflix docuseries called Dancing for the Devil: The 7M TikTok Cult has brought this form of coercive control back into the spotlight. The 3-part series on the 7M cult explores how a group of young TikTok dancers allegedly fell under the influence of a church pastor who also became their talent manager and siphoned off most of their income. Some former members of the group also filed police reports of continuing sexual abuse. These wild tales can make you wonder how anyone can fall under the spell of a charismatic cult leader. In some cases, it leads to victim blaming. But research shows that powerful cult leaders are highly adept at using psychological manipulation to control followers. Cult members typically don’t realize they are being brainwashed. If you suspect that you or someone you love may be in a similar situation, it’s important to recognize the signs of a cult. This blog will introduce you to the warning signs of a cult as well as the steps to take to leave a cult and rebuild your life. Research shows that powerful cult leaders are highly adept at using psychological manipulation to control followers. Cult members typically don’t realize they are being brainwashed.WHAT IS A CULT?
Experts continue to search for a standard cult definition. In general, a cult is a group of people who are typically controlled by a self-appointed, charismatic leader. In general, the cult leader uses psychological manipulation tactics and coercive control to dominate cult members. The foundation of a group’s ideology may be rooted in a variety or areas, such as:- Religious beliefs
- Political theories
- Philosophical concepts
- Lifestyle activities
12 WARNING SIGNS OF A CULT
There are many signs that an organization may be a cult. Some of the following signs come from the Cult Education Institute while others are based on the work of cult researchers. Here are 12 warning signs of a cult:- The truth: In cults, there’s a belief that the leader exclusively knows the “truth”—some transcendent concept that provides a solution for people’s biggest problems and fears.
- Love bombing: Cults often shower new recruits with love, a sense of community, a place to live, and a sense of hope and purpose.
- Thought reform: A 2022 study shows that cult leaders use various forms of mind control to influence followers and get them to adopt shared beliefs and values.
- Authoritarianism: The leader makes all rules and has undue influence over all aspects of members’ lives—finances, relationships, living situations, and more. This control comes without any sort of accountability for the leader.
- No questions allowed: There is usually a lack of tolerance for criticism of or questions about the group or leader. There is a firm belief that the leader or group is right about everything.
- Financial control: The leader or group maintains complete control over the financial budget and expenses without providing any statements to members.
- Fear factor: The leader or group instills irrational fears about the outside world, such as anxiety about conspiracies, impending disasters, eternal damnation, or persecution.
- Need to improve: Members believe they are incapable of ever being “good enough” yet are constantly seeking validation from the leader. This can lead to toxic perfectionism.
- Leaving is forbidden: In cults, there is no valid reason why any member would leave, and there’s a belief that any member who does leave is wrong or even evil.
- Abuse is common: Followers may experience various forms of abuse and may face threats of physical harm, shunning, and other forms of punishment.
- Gaining attention: Abuses may have been documented in the media or investigated by law enforcement. This is viewed as persecution by the outside world and increases an us-vs-them mentality.
- Blackmail: Members may be coerced into proving their loyalty by engaging in acts that are illegal or immoral. Then the group uses that information as blackmail that will be leaked if the follower attempts to leave.
HOW TO KNOW IF SOMEONE IS IN A CULT
When someone joins a cult, it can be difficult for friends and family members to realize it. It can also be challenging for individuals themselves to accept that their newfound community is actually a cult. Here are some of the ways to know that someone is a member of a cult.- Members tend to exhibit a sudden and extreme devotion to the leader or group, dropping previously held beliefs and values.
- Members often live together in communal housing.
- As a follower’s involvement deepens, their personal identity starts to blend and blur with that of the leader, the group, and/or God.
- Followers refuse to respond to any criticism or questions about the leader or group, viewing it instead as “persecution” of the group or leader.
- People start using jargon, speech patterns, and mannerisms specific to the group. This can sound like the person is reading from a script.
- Members seem to lose the ability to think independently while increasing reliance on the leader or group to solve problems.
- Followers tend to lose interest in past goals and hobbies, replacing them with an extreme focus on the objectives of the leader or group.
- A significant decrease in sense of humor and a loss of the ability to do anything on the spur-of-the-moment.
- People in cults tend to isolate themselves from former friends and family and may become secretive about activities related to the group or leader.
- People find ways to justify the leader’s or group’s actions regardless of how cruel, hard-hearted, or severe they may seem.
- Individuals avoid former members, viewing them as bad, evil, or wrong.
WHO JOINS A CULT?
Cults typically prey upon people who are in vulnerable situations. For example, they may target any of the following:- Drug and alcohol addicts
- Teenage runaways
- People who have lost a loved one
- Physical, sexual, or emotional trauma survivors
- People in new situations (such as college students)
- People struggling with mental health disorders, such as anxiety disorders and clinical depression
HOW TO GET OUT OF A CULT
Leaving a cult can be challenging on many levels. You may lack a support network outside the group, financial resources, or a place to stay. Steps that can help you remove yourself from a cult including the following:- Gain awareness: Recognizing the signs of a cult is the first step in gaining the motivation to leave. For example, do you feel like you’re being controlled? Are you being coerced to engage in activities that make you feel uncomfortable? Are you or others in your group being harmed physically, financially, sexually, or emotionally?
- Connect with support: If you’re able to, reconnect to people you trust or reach out to mental health professionals who are outside of the cult. They can provide you with emotional support and may be able to help you when you’re ready to leave.
- Make a plan to leave: Decide on a time when you can exit the cult, keeping your physical safety in mind. For some people, this may take a while, so you may have to go through the motions for some time. In other cases, you may want to depart quickly.
- Know where you’ll stay: Find a safe and secure place you can stay at first. Check with family or trusted friends to see if you can stay with them for a while.
- Leave: When the time comes, leave. Be aware that you may need to sneak out secretly, leave personal belongings behind, or leave without saying goodbye to the people you love.
- Recover: Rebuilding your life can be challenging. Finding new friends, a job, and a new daily routine can be stressful. Research on former cult members shows that you may feel confused as you try to reconnect with your own identity, personal values, and beliefs.
WHAT IS THE CENTRAL EXECUTIVE NETWORK?
The central executive network, also known as the frontoparietal network (FPN), is a team of brain regions that work together to control and manage your thoughts and actions. It includes areas such as:- Parts of the frontal lobe, which is located at the front of your brain
- Parietal lobe, found on the top and back of your brain
- Concentration—helping you stay focused on important tasks
- Working memory—a form of short-term memory that involves holding information in your mind for a brief time while you manipulate it
- Decision-making—making choices that fit with your goals
- Problem-solving—following rules that help you solve complex issues
- Information processing—integrating data from external and internal sources
- Task switching—shifting attention from one task to another when necessary
THE CEN’S ROLE IN EVERYDAY LIFE
Every day, you face situations that require focus and decision-making. Whether you’re solving math problems, writing an essay, or playing a sport, the CEN helps you stay on track. The CEN is also at work when you need to pay attention on a Zoom meeting, remember instructions from your supervisor, or even resist the urge to check your phone while on the job. It’s like having a coach in your brain that pushes you to concentrate and keeps you from getting distracted.HOW THE CENTRAL EXECUTIVE NETWORK AFFECTS MENTAL HEALTH
The central executive network doesn’t just help you with work and school. It also plays a significant role in your mental health. Let’s look at how the CEN influences various aspects of mental well-being:- Stress and Anxiety: When you’re stressed or anxious, the CEN helps you manage those feelings by focusing your mind on solutions or calming techniques. However, if the CEN is overwhelmed, it might be harder for you to cope with everyday stress, leading to more anxiety.
- Depression: In some cases of depression, the CEN might not function as effectively. This can make it hard for someone to concentrate or make decisions, which are common challenges for those experiencing clinical depression.
- ADHD: Attention-deficit/hyperactivity disorder (ADHD), also known as attention-deficit disorder (ADD), is often linked to difficulties with the CEN. People with ADHD might find it hard to focus, control impulses, or plan ahead because their central executive network isn’t coordinating their brain’s activities as smoothly as it should.
SUPPORTING THE CENTRAL EXECUTIVE NETWORK FOR BETTER MENTAL HEALTH
Knowing how important the CEN is, it’s critical to support it. Emerging research shows that there are ways to strengthen this brain network, which can help improve mental health:- Mindful Activities: Practices like mindfulness or meditation can train your brain to use the CEN more effectively. These activities help you learn to control your attention and manage distractions.
- Regular Exercise: Physical activity is not just good for your body; it’s also great for your brain. Exercise can enhance the functioning of the CEN, making it easier to focus and solve problems.
- Healthy Sleep Habits: Getting enough sleep is crucial for the CEN. A well-rested brain performs better, especially when it comes to tasks that require attention and executive control.
- Problem-Solving Games: Engaging in activities that challenge your brain, like puzzles or strategy games, can also strengthen the CEN. These fun activities make you think critically and keep your decision-making skills sharp.
