

Depression
Depression isn’t a single or simple disorder. At Amen Clinics, we go beyond traditional mental health care by using brain imaging to identify your unique type of depression for more targeted and effective treatment.
WHAT IS DEPRESSION?
Depression (known as clinical depression or major depressive disorder) is one of the most common mental health problem in the nation and across the globe. Everybody gets the blues from time to time. For most of us, we bounce back from these low moods and get back to enjoying our lives. For some people, however, the sense of sadness, emptiness, or hopelessness doesn’t dissipate, and it begins to affect how you think, how you feel, and how you act. When these feelings persist, this mood disorder can interfere with daily life and that can lead to psychological and physical issues.
Who GETS DEPRESSION?
Approximately 17.3 million people in America are affected by depression, representing over 7% of the adult population. The condition is more common in females, who are twice as likely as men to suffer a depressive episode. Research shows the condition is rising most rapidly among teens and young adults. About 36% of girls will experience clinical depression during their teenage years compared to 13% of teenage boys.

COMMON Symptoms OF DEPRESSION
- A persistent feeling of sadness, anxiety, or emptiness
- A loss of interest in activities that were previously enjoyable
- Feeling tired or having a lack of energy
- Having trouble sleeping, waking up too early, or oversleeping
- Changes in appetite or unplanned weight loss or gain
- Aches, pains, headaches, cramps, or digestive issues without an obvious physical cause

UNTREATED DEPRESSION INCREASES THE RISK OF:
- Substance Abuse
- Relationship Problems
- Work Problems
- Heart Disease
- Suicide

Consequences of Untreated Depression
It is estimated that nearly 2 out of every 3 people struggling with depression don’t seek or receive treatment for their condition. When left untreated, depression can ruin your life. Clinical depression increases the risk of substance abuse, destroys relationships, interferes with your ability to excel at work, and makes you more vulnerable to certain medical conditions. For example, people with depression are more likely to develop heart disease and are more likely to die following a heart attack than people without the condition. Even more troubling is the fact that depression is the cause of two-thirds of suicides.

Why Choose Amen Clinics for DEPRESSION Treatment?
It is not uncommon for depression to be misdiagnosed for another mood disorder, such as bipolar disorder, or for other conditions like ADD/ADHD, or even dementia. Getting the wrong diagnosis and the wrong treatment can make your symptoms worse and keep you in a downward spiral. Our brain-imaging work allows us to distinguish depression from other conditions and to identify any co-existing issues that also need to be treated. Brain imaging has taught us that depression is not a single or simple disorder, and that giving everyone who’s depressed the same medication will never work. Based on your brain scans, we can better determine how you will respond to treatment so you can feel better faster.
DEPRESSED Brains Work Differently
Brain-imaging studies show that depression is not a character flaw or personal weakness. It is associated with biological changes in the brain. People with depression often have too much activity in the deep limbic system—the brain’s emotional center. But not everyone with depression has the same underlying brain patterns. Brain imaging has taught us that there are 7 different brain patterns associated with depression, and knowing your type can be the key to getting the most effective treatment.
SPECT (single photon emission computed tomography) is a nuclear medicine study that evaluates blood flow and activity in the brain. Basically, it shows three things: healthy activity, too little activity, or too much activity. A healthy “active” scan shows the most active parts of the brain with blue representing the average activity and red (or sometimes red and white) representing the most active parts of the brain. In the healthy scan on the top right, the most active area is in the cerebellum, at the back/bottom part of the brain. The brain scan below it shows overactivity in the deep limbic system (the brain’s emotional center), a pattern commonly seen in depression.
Healthy Brain Scan
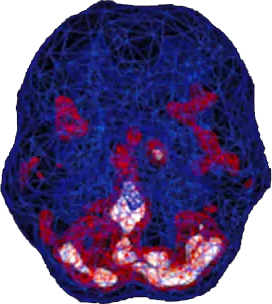
Depressed Brain Scan
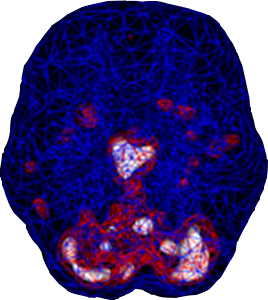
THE 7 TYPES OF DEPRESSION AND ANXIETY
Our brain imaging work at Amen Clinics has helped us identify 7 different brain patterns associated with depression. And each type requires its own treatment plan.
This section provides greater detail about each of the seven types.
Type 1: Pure Anxiety
Since depression and anxiety are often co-occurring disorders, we include anxiety as one of the seven types of depression. Pure Anxiety often results from too much activity in the basal ganglia, setting one’s “idle speed” on overdrive.
Common symptoms of Pure Anxiety include:
- Frequent feelings of nervousness or anxiety
- Panic attacks
- Avoidance of people or places due to a fear of having anxiety or panic attacks in public
- Symptoms of heightened muscle tension (headaches, sore muscles, hand tremor)
- Periods of heart pounding, nausea, or dizziness
- Tendency to predict the worst
- Multiple persistent fears or phobias (such as dying or doing something crazy)
- Conflict avoidance
- Excessive fear of being judged or scrutinized by others
- Being easily startled or a tendency to freeze in anxiety-provoking or intense situations
- Shyness, timidity, and getting easily embarrassed
- Biting fingernails or picking skin
Type 2: Pure Depression
Pure Depression often results from excessive activity in the deep limbic system—the brain’s emotional center. People with this depression type struggle with depressive symptoms that range from chronic mild sadness (dysthymia) to crippling major depression, where it’s difficult to even get out of bed.
Common symptoms of Pure Depression include:
- Persistent sad or negative mood
- Loss of interest in usually pleasurable activities
- Restlessness, irritability, or excessive crying
- Feelings of guilt, worthlessness, helplessness, hopelessness, or pessimism
- Sleeping too much or too little, or early-morning awakening
- Appetite changes and/or weight loss or weight gain
- Decreased energy or feeling “slowed down”
- Thoughts of death or suicide, or suicide attempts
- Difficulty concentrating, remembering, or making decisions
- Persistent physical symptoms (such as headaches, digestive problems, or chronic pain)
- Chronic low self-esteem
- Persistent feeling of being dissatisfied or bored
Type 3: mixed depression/anxiety
Mixed Depression and Anxiety involves a combination of both Pure Anxiety symptoms (listed above) and Pure Depression symptoms (listed above). This type shows excessive activity in the brain’s basal ganglia and the deep limbic system. One type may predominate at any point in time, but symptoms of both are present on a regular basis.
Type 4: Over focused Depression/Anxiety
Overfocused Depression and Anxiety involves excessive activity in the brain’s anterior cingulate gyrus, basal ganglia, and/or the deep limbic system. People with this type—which occurs more frequently in the children or grandchildren of alcoholics—have trouble shifting attention and often get locked into anxious and/or negative thoughts or behaviors. This can look like:
- Obsessive-compulsive disorder (stuck on negative thoughts or actions)
- Phobias (stuck on a fear)
- Eating disorders (stuck on negative eating behavior)
- Posttraumatic stress disorder or PTSD (stuck on a past traumatic event)
Common symptoms of Overfocused Depression/Anxiety include four symptoms from Pure Anxiety (listed above) and/or Pure Depression (listed above), plus at least four of the following:
- Excessive or senseless worrying
- Upset when things are out of place or things don’t go the way you planned
- Tendency to be oppositional or argumentative
- Tendency to have repetitive negative or anxious thoughts
- Tendency toward compulsive or addictive behaviors
- Intense dislike for change
- Tendency to hold grudges
- Difficulty seeing options in situations
- Tendency to hold onto own opinion and not listen to others
- Needing to have things done a certain way or you become upset
- Others complain you worry too much
- Tendency to say “no” without first thinking about the question
Type 5: Temporal Lobe Depression/Anxiety
Temporal Lobe Depression and Anxiety is related to too little or too much activity in the temporal lobes (involved in moods, emotions, and memory), in addition to overactivity in the basal ganglia and/or deep limbic system.
Common symptoms of Temporal Lobe Depression/Anxiety include four symptoms from Pure Anxiety (listed above) and/or Pure Depression (listed above), plus at least four of the following:
- Short fuse or periods of extreme irritability
- Periods of rage with little provocation
- Often misinterpreting comments as negative when they are not
- Periods of spaciness or confusion
- Periods of panic and/or fear for no specific reason
- Visual or auditory changes, such as seeing shadows or hearing muffled sounds
- Frequent periods of déjà vu
- Sensitivity or mild paranoia
- Headaches or abdominal pain of uncertain origin
- History of head injury
- Family history of violence or explosiveness
- Dark thoughts that may involve suicidal or homicidal thoughts
- Periods of forgetfulness or memory problems
Type 6: Cyclic Depression/Anxiety
Cyclic Depression and Anxiety is associated with extremely high activity in the brain’s basal ganglia and/or deep limbic system. These areas of excessive activity act like “emotional seizures” as the emotional centers hijack the brain for periods of time in a cyclical pattern. Cyclical disorders, such as bipolar disorder, cyclothymia, premenstrual tension syndrome, and panic attacks are part of this category because they are episodic and unpredictable.
Common symptoms of Cyclic Depression/Anxiety include four symptoms from Pure Anxiety (listed above) and/or Pure Depression (listed above) plus periods of time with at least four of the following:
- Abnormally elevated, depressed, or anxious mood
- Decreased need for sleep, feeling energetic on dramatically less sleep than usual
- Grandiose notions, ideas, or plans
- Increased talking or pressured speech
- Racing thoughts
- Markedly increased energy
- Poor judgment leading to risk taking behavior (departure from usual behavior)
- Inappropriate social behavior
- Irritability or aggression
- Delusional or psychotic thinking
Type 7: Unfocused Depression/Anxiety
Unfocused Depression and Anxiety is associated with low activity in the prefrontal cortex (PFC) in addition to high activity in the basal ganglia and/or deep limbic system. The PFC is involved with attention, focus, impulse control, judgment, organization, planning, and motivation. When the PFC is underactive, people often have problems with these executive functions.
Distinguishing Unfocused Depression and Anxiety from ADHD can be difficult because of the similarity in symptoms. However, brain imaging provides a window into the brain to see the areas with too little or too much activity. This allows for a more accurate diagnosis.
Symptoms of Unfocused Depression/Anxiety include at least four items from the Pure Anxiety (listed above) and/or Pure Depression symptoms (listed above), plus at least four of the following:
- Trouble staying focused
- Spaciness or feeling in a fog
- Overwhelmed by the tasks of daily living
- Feeling tired, sluggish, or slow moving
- Procrastination, failure to finish things
- Chronic boredom
- Distractibility
- Forgetfulness
- Difficulty expressing feelings
- Lack of empathy for others
A variation of Unfocused Depression/Anxiety is caused by overall reduced blood flow and activity in the cortex along with too much activity in the basal ganglia and/or deep limbic system. This pattern may be related to physical illness, drug or alcohol abuse, hypoxia (lack of oxygen), infections (such as Lyme disease or COVID-19), traumatic brain injury, or exposure to toxic mold or other environmental toxins. Symptoms of this variation also include frequent feelings of sickness, mental dullness, “brain fog,” or cognitive impairment.
DEPRESSION TESTIMONIALS
WANT TO LEARN MORE? DOWNLOAD OUR ANXIETY & DEPRESSION TYPES EBOOK






