

Suicidal Thoughts & Behavior
Suicidal thoughts and behaviors are serious warning signs of emotional distress that should never be ignored. At Amen Clinics, we go beyond traditional mental health care with advanced brain imaging to uncover underlying brain dysfunction and co-occurring mental health conditions—leading to more accurate diagnoses and potentially life-saving, personalized treatment.
What are Suicidal Thoughts and Behavior?
Everybody struggles in life. It’s normal to feel sad, anxious, and stressed-out from time to time. However, if feelings of deep depression, despair, overwhelming anxiety, or a persistent sense of failure become the constant backdrop to your life, you may start thinking your situation is hopeless and there is no way out. The downward spiral may eventually lead to thoughts of suicide or suicidal behavior, which includes talking about suicide, planning how to do it, or taking action to end your life. For every suicide there are an estimated 25 suicide attempts. If you or a loved one has experienced suicidal thoughts or behavior, there’s one very important thing you need to know: Help is available!
WHO HAS SUICIDAL THOUGHTS AND BEHAVIOR?
Every day, approximately 135 people in the U.S. die by suicide, making it the 12th leading cause of death. Among people aged five to 24, suicide is the second leading cause of death. And it ranks as the fourth leading cause of death for those between 25 and 44 years of age. In 2022, twice as many Americans died by suicide than by homicide.
People of any age, gender, or ethnicity can struggle with thoughts of taking their own life. Men are more likely to die by suicide, but women are three times more likely to attempt suicide.

WHAT CAUSES SUICIDAL THOUGHTS AND BEHAVIORS?
Research indicates that having a genetic risk for depression is one of the biggest underlying factors for suicide attempts. There are numerous situations and experiences that might lead to feelings of hopelessness, shame, guilt, or other painful emotions and increase suicidal thoughts and actions. These include (but are not limited to):
- Being bullied
- Chronic stress
- Family rejection
- Social isolation
- Substance abuse
- Traumatic brain injury (TBI)
- Chronic medical conditions
- Family history of suicide
- History of trauma or abuse
- Family history of substance abuse
- Family history of mental health problems
- Mental health disorders (especially depression)
- Exposure to the suicidal behavior of a family member or friend or even in media

WARNING SIGNS OF SUICIDE
- Talking about feeling hopeless
- Talking about being in pain
- Talking about being a burden
- Increasing the use of drugs or alcohol
- Sleeping too little or too much
- Extreme mood swings
- Talking about seeking revenge
- Withdrawing socially
- Showing rage

Why Choose Amen Clinics for TREATING SUICIDAL THOUGHTS AND BEHAVIOR?
Depression, anxiety disorders, posttraumatic stress disorder (PTSD), anorexia nervosa, and other mental health issues can be major contributors to suicidal ideation and behavior, especially when these conditions go untreated or are misdiagnosed. Unfortunately, this is far too common in people who are suffering with symptoms of psychiatric disorders. At Amen Clinics, our brain-imaging work using SPECT technology has shown that suicidal thoughts and behavior can have multiple contributing factors. Scanning the brain can provide vital information so our doctors can create a personalized treatment plan to help suicidal patients get better.
SUICIDAL Brains Work Differently
Our brain-imaging work has taught us so much about the brains of people who have suicidal thoughts and behaviors. We have scanned over 300 people who have attempted suicide and many more who have thought about ending their life. The majority of these people had a tendency to get stuck in negative thinking patterns, were impulsive, were prone to anger and irritability, and showed poor judgment. The combination of negative thoughts, anger, and impulsivity can add up to a dangerous situation.
SPECT (single photon emission computed tomography) is a nuclear medicine study that evaluates blood flow and activity in the brain. Basically, it shows three things: healthy activity, too little activity, or too much activity. The healthy surface brain SPECT scan on the top right shows full, even symmetrical activity. The scan below it of someone who attempted suicide reveals low blood in several areas of the brain, including the prefrontal cortex, which is involved in impulse control, judgment, and decision-making. See below for more about common SPECT findings in suicidal people.
Healthy Brain Scan
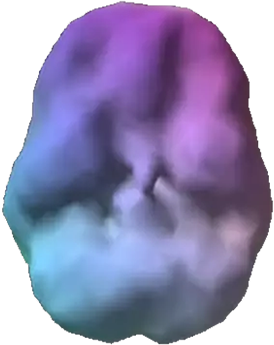
Suicidal Brain Scan
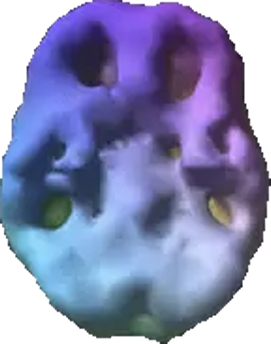
Suicide and Mental Health
Before coming to Amen Clinics, many of our patients have already seen other providers and tried a number of different treatments, yet their symptoms persisted. In part, this is because several mental health conditions are not single or simple disorders. Over the past three decades, our brain-imaging work has taught us that anxiety, depression, addiction, attention deficit hyperactivity disorder (ADHD), also known as attention deficit disorder (ADD), and other conditions have multiple types. We have identified seven types of anxiety and depression, seven types of ADHD/ADD, and more. To get relief, you need to know your type.
For people who are suffering from suicidal depression, severe anxiety, or other mental health issues, scanning the brain can provide vital information.
Is Self-Harm A Warning Sign of Suicide?
You may think that other types of self-inflicted injury—such as cutting, burning, or head banging—might be a sign of suicidal behavior. Although causing intentional physical harm to oneself is very troubling behavior, it is generally carried out as a maladaptive coping mechanism for dealing with a painful aspect of life rather than an attempt to end one’s life. Self-harm is considered nonsuicidal in nature; however, up to 40 percent of people who self-harm think about suicide, and approximately 50-85 percent have made at least one suicide attempt in their lifetime. Because of this, it is absolutely critical to seek help for any form of self-harming behavior. These behaviors can also be a sign of other mental health conditions, such as depression, bipolar disorder, anxiety disorders, borderline personality disorder, and obsessive-compulsive disorder, which is why they need to be evaluated and treated.
Suicidal Thoughts and Behavior and the Brain
As mentioned above, Amen Clinics has scanned more than 300 patients who have attempted suicide and many more who have thought about taking their own life. The SPECT scans of these patients revealed abnormalities in the brain, especially in these areas:
- Temporal Lobes: Brain SPECT imaging shows that people with suicidal thoughts and suicide attempts often have abnormalities in the left temporal lobe. In an Amen Clinics study, we saw left temporal lobe problems in 62 percent of our patients who had serious suicidal thoughts or behaviors.
- Traumatic Brain Injury (TBI): After reviewing nearly 300,000 functional brain scans related to behavior it is clear that head injuries are a leading cause of mental health issues, such as depression, anxiety disorders, panic disorder, PTSD, ADHD/ADD, substance abuse, psychosis, borderline and antisocial personality disorders, dementia, and aggression. Concussions and TBIs also increase the risk of suicide. When the brain has functional damage due to a head injury, it’s critical to heal the brain in order to overcome any mental health problems. At Amen Clinics, 40 percent of our patients have had a significant brain injury.
- Prefrontal Cortex: A large-scale study by researchers at Portland State University found that about 22 percent of people who died by suicide were legally intoxicated at the time of their death. Brain scans show that alcohol lowers function in the prefrontal cortex, a brain region involved in impulse control, judgment, and decision-making.
- Anterior Cingulate Gyrus: People with overactivity in this area of the brain tend to get stuck on negative thoughts, which is one of the traits we see in people with suicidal thoughts and behavior.


