ARCHIVE
Some anxiety is good for you. It’s true! Our brains are biologically wired to protect us from danger, and a healthy dose of anxiety helps to keep us safe. It also keeps us motivated and prepared, so we can perform at a high level. Unfortunately, there are millions of people suffering with far too much anxiety. They can spend time predicting the worst, being wracked by nervousness, chronic muscle tension, among other symptoms. It’s as though their “idle” is set too high, and they’re frequently plagued by self-doubt, fear, and panic. In some cases, it can lead to an anxiety attack or panic attack. If you’re one of the millions of Americans struggling with anxiety or panic, the good news is that you can gain control of your symptoms. If you experience an anxiety attack or a panic attack, simply follow this 4-step plan. It’s the same one Dr. Daniel Amen has taught to thousands of his own patients at Amen Clinics. Click to Tweet If you’re one of the millions of Americans struggling with anxiety or panic, the good news is that you can gain control of your symptoms. Simply follow Dr. Amen’s 4 step panic plan.AMEN’S 4-STEP PANIC PLAN
Here are 4 steps to help you break an anxiety attack or panic attack.Step 1: Do diaphragmatic breathing.
Often when people begin to experience anxiety, their breathing becomes shallow, rapid, and erratic. Since the brain is the most metabolically active organ in your body, any state that lowers oxygen will trigger more fear and panic. By taking slow, deep breaths you’ll boost oxygen to your brain and start to regain control over how you feel. One way to practice deep breathing is by learning how to breathe from your diaphragm—the area of the body that tends to get “clenched” when we’re anxious. To practice breathing from your diaphragm, try this:- Lie on your back and place a small book on your belly.
- As you slowly inhale through your nose, make the book go up. Hold your breath at the top of your inhalation for 2 seconds.
- When you exhale, make the book go down and then hold your breath for 2 seconds before inhaling again.
- Repeat 10 times and notice how relaxed you feel.
Step 3: Write down your thoughts.
Often in panicked situations, our thoughts become distorted and need to be challenged. Pay attention to the automatic negative thoughts (ANTs) in your mind and write them down to see if they make sense. The act of writing them down helps get them out of your mind. Then question those thoughts to see if they are distorted. Ask yourself if your thoughts are true. Then notice how these thoughts make you feel. Chances are, ANTs make you feel more anxious and panicky. They may make your heart race, cause your breathing to become more shallow, or make your stomach feel like it’s tied up in knots. Take note of all these sensations. Then challenge yourself to come up with a more realistic version of the thought. Or ask yourself if the opposite of that though is actually truer than the original thought. Look for evidence to support this new thought. When you catch yourself in the middle of an ANT invasion, taking a logical approach to eliminating those ANTs can help you calm down.Step 4: Supplement your brain and body.
If you’ve practiced steps 1-3, but are still suffering from too much anxiety, you may need supplements or medication to help you feel calmer. Remember that this is the last step—to be used if the first 3 aren’t effective. Some people with severe symptoms may require some form of anxiety medication on a temporary basis. Be sure to check with your health care provider before taking any form of anti-anxiety medication and be aware of the risks. For example, functional brain imaging with SPECT scans shows that anxiety drugs can have harmful effects on the brain when taken over time. Benzodiazepines decrease activity in the brain and increase the risk of dementia, including Alzheimer’s disease. Below are images of a healthy SPECT scan and a scan of someone who was hooked on benzodiazepines. In the healthy scan, there is full, even, symmetrical activity. In the benzodiazepine scan, there are many “holes” that indicate low levels of blood flow and activity. The bumpy, scalloped appearance is similar to what is seen in SPECT scans of people who are alcoholics or who have brain toxicity. Healthy SPECT Surface Scan Full, even, symmetrical activity
Benzodiazepine Image
Full, even, symmetrical activity
Benzodiazepine Image
 Overall decreased activity
Some individuals do well with nutritional supplements. Calming nutraceuticals include magnesium, GABA, ashwagandha, and some of the B vitamins, especially B6. Taking these on a daily basis may have a beneficial effect.
Overall decreased activity
Some individuals do well with nutritional supplements. Calming nutraceuticals include magnesium, GABA, ashwagandha, and some of the B vitamins, especially B6. Taking these on a daily basis may have a beneficial effect.
CONQUERING ANXIETY AND PANIC
By following these 4 simple steps, you can regain control over your panic attacks and anxiety disorders. Make it a priority to practice these steps on a regular basis, and you should notice a decrease in anxiety symptoms. Anxiety attacks, panic attacks, and other mental health issues can’t wait. At Amen Clinics, we’re here for you. We offer in-clinic brain scanning and appointments, as well as mental telehealth, clinical evaluations, and therapy for adults, teens, children, and couples. Find out more by speaking to a specialist today at 888-288-9834 or visit our contact page here. Most individuals know that it’s important to treat strep throat. If it remains untreated, it can eventually lead to rheumatic heart disease or congestive heart failure. But that’s not all. There are several mental health consequences that most people are unaware of, and they can greatly impact a child’s life. Look at Henry, for example. At age 10, Henry was struggling with anxiety, depression, ADD/ADHD, and Tourette’s (a tic disorder). He was taking three psychiatric medications to cope with these mental health conditions. His parents, who were going through a divorce, initially blamed his symptoms on the family stress. But his grandfather had been a patient at Amen Clinics, and he encouraged them to schedule a visit for Henry to get a brain SPECT scan. That brain scan revealed something Henry’s previous physicians had never considered: PANS/PANDAS. If a child has PANS/PANDAS, there is hope for healing. First, it’s critical to get tested for common infections. In addition, brain imaging with SPECT scans can offer invaluable information that leads to a more accurate and complete diagnosis.WHAT IS PANS/PANDAS?
Over two decades ago, the National Institute of Mental Health (NIMH) issued a report saying that strep throat could cause the sudden onset of OCD and Tourette’s in kids, adolescents, and teens. They called this new syndrome pediatric autoimmune neuropsychiatric disorders associated with strep (PANDAS). Neuroscientists eventually realized that strep throat is not the only infectious disease that can lead to mental health issues. Because of this, they began labeling the condition PANS (pediatric acute-onset neuropsychiatric syndrome). The onset of this syndrome can occur rapidly. According to Dr. Susan Swedo at the National Institute of Mental Health, “Parents will describe children with PANS as overcome by a ‘ferocious’ onset of obsessive thoughts, compulsive rituals, and overwhelming fears. Clinicians should consider PANS when children or adolescents present with such acute-onset of OCD or eating restrictions in the absence of a clear link to strep.”SIGNS AND SYMPTOMS OF PANS/PANDAS
Henry’s symptoms are some of the most common signs of PANS/PANDAS. However, it’s important to understand that this condition can cause a wide variety of emotional and behavioral symptoms, such as:- Obsessive thoughts and compulsive behaviors (commonly seen in OCD)
- Severe anxiety
- Panic attacks
- Phobias
- Attention problems and/or hyperactivity (commonly seen in ADD/ADHD)
- Tics (motor or vocal)
- Restrictive eating habits
- Oppositional behavior (commonly seen in oppositional defiant disorder or ODD)
- Depression or moodiness
- Aggression or anger
- Sensory sensitivities
PANS/PANDAS AND THE BRAIN
Functional brain-imaging shows that PANS/PANDAS affects the way the brain functions. SPECT is a functional brain-imaging technology that measures blood flow and activity in the brain. It shows areas of the brain with healthy activity as well as areas with underactivity or overactivity. Henry’s SPECT scan revealed overactivity throughout his brain, a pattern that is consistent with inflammation. Additional testing confirmed that the youngster had Lyme disease as well as PANDAS. Healthy Active SPECT Scan An “active” SPECT scan shows the areas of the brain with the most activity, which are seen in white in this image. In the healthy brain, the most active area is in the cerebellum at the back/bottom part of the brain. Henry’s Active SPECT scan Overall increased activity, looking inflamedINFECTIONS AND MENTAL HEALTH PROBLEMS
PANS/PANDAS can be caused by numerous infections, including:- Strep throat
- Borrelia burgdorferi (Lyme disease)
- Mycoplasma pneumoniae (walking pneumonia)
- Herpes simplex
- Common cold
- Influenza
- Mononucleosis
- Epstein-Barr
HEALING FROM PANS/PANDAS
If a child has PANS/PANDAS, there is hope for healing. First, it’s critical to get tested for common infections. In addition, brain imaging with SPECT scans can offer invaluable information that leads to a more accurate and complete diagnosis. Seeing an integrative medicine (also called functional medicine) physician can be helpful in order to diagnose and effectively treat any underlying infections.Medical treatments for PANS/PANDAS include:
- Medications: Antibiotics, anti-inflammatory medications, and steroids may be prescribed.
- Intravenous immunoglobulin (IVIG): IVIG is a treatment in which human antibodies are delivered intravenously. In one study published in The Lancet, this treatment resulted in a 45% reduction in symptom severity in children with PANS/PANDAS after just one month.
- Plasmapheresis: This treatment involves separating plasma from blood with a machine then returning the blood to the patient. According to the same study from The Lancet mentioned above, plasma exchange led to a 58% decrease in the severity of PANS/PANDAS symptoms.
Natural treatments for PANS/PANDAS include:
- Elimination diet: Research shows that poor gut health may play a role in PANS/PANDAS. For this reason, supporting gut health is crucial. For 30 days, eliminate the following potential allergens from your child’s diet: gluten, dairy, sugar, soy, corn, artificial dyes, additives, and preservatives. See if there is any improvement in their symptoms. Then gradually reintroduce foods one by one to see if they trigger reactions.
- Avoiding environmental toxins: Experts suggest that mold, chemicals in common household cleaners, smoke, volatile organic compounds (VOCs) in rugs and carpeting, and other toxins found in homes can contribute to PANS/PANDAS symptoms. Removing any toxins from your home may benefit a child with this condition. For example, avoid harsh chemical cleaners, choose personal care products that are free of toxic chemicals, and consider removing carpeting or rugs, if necessary.
- Stress-management techniques: Teaching a child with PANS/PANDAS to self-soothe can be a powerful tool. Specific techniques that calm stress include deep belly breathing, listening to calming music, prayer or meditation, and warming the hands with the mind. One of the easiest stress busters for kids is laughter. To spark laughter, watch a comedy or look at a few funny videos online with them.
- Nutraceuticals: Research shows that kids with PANS/PANDAS may be lacking in key nutrients, so it’s important to take a multivitamin/mineral. As an example, a 2018 study found reduced levels of vitamin D in children with the syndrome. Taking a vitamin D supplement to optimize levels is recommended. Other supplements that support the brain and gut include omega-3 fatty acids and probiotics.
Is Your Child Struggling with Mental Health Issues?
Have you been working diligently to put proven parenting strategies into practice? Despite this, is your child is still misbehaving, creating conflict, lacking motivation, procrastinating, underperforming at school, having trouble making friends, or having other problems? If so, a mental health issue may be the culprit. When parenting strategies aren’t working, a childhood mental health issue may be the culprit.KIDS AND MENTAL HEALTH PROBLEMS
Mental health problems and learning disorders—all of which are actually brain health issues—are rising among the more than 73 million kids ages 0 to 17 in the US. Just look at these statistics:- 75% of all mental health issues begin before age 25.
- 50% of children who struggle with mental health issues are unidentified and receive no treatment.
- 46% of students with a mental health issue drop out of school.
- 65–75% of jailed teens have a mental illness, including brain injuries.
- Suicide is the second leading cause of death, behind accidents, among teens ages 15 to 19.
- 86% of teens know someone with a mental health issue.
- Over 86% of teens say mental health is an important topic.
- Over 84% say there is a stigma surrounding mental health.
WHY PARENTS MISS MENTAL HEALTH ISSUES IN KIDS
This is not surprising because most parents aren’t experts in the differences between “normal” and “abnormal” behaviors, emotional health, or brain and mental wellness. Parents are usually only exposed to their own children, their nieces and nephews, and their kids’ friends. So, when a youngster seems consistently down in the dumps, constantly worries, or acts aggressively, it’s natural to assume it’s just your child’s nature or that they have an attitude problem. If you misread an underlying brain health problem or mental health issue as an attitude issue, your knee-jerk reaction may be to increase discipline and consequences, which may be harmful. Many kids who have brain/mental health problems are actually trying hard to do what Mom and Dad ask, but they just aren’t able to do it because of the way their brain is wired. If your child is consistently struggling at school, routinely having trouble getting along with others, or frequently losing their temper, take a moment and ask yourself, “Could this be a sign of something else?”WHEN TO SEEK HELP FOR YOUR CHILD’S MENTAL HEALTH
If you have a feeling that your youngster or adolescent may have a behavioral, emotional, or learning issue, don’t wait. Bring up any concerns with your child’s pediatrician or other healthcare provider. Small issues that remain untreated can morph into big problems. On the flip side, early intervention can put a halt to unwanted issues and can improve your child’s future. In some cases, simple lifestyle changes or nutritional supplements may be all they need. If you’re noticing problematic behaviors or emotional issues, it’s important to get your child on a brain-healthy program sooner rather than later. When these issues remain untreated, they can have lifelong consequences that make parenting exponentially more difficult. In the short term, these issues are associated with increased family discord, academic underachievement, and more. Over time and into adulthood, they are linked with increased risks of school dropouts, traffic accidents, substance abuse, job failure and unemployment, financial problems, obesity, divorce, and suicidal thoughts and behaviors. After working with thousands of children, we can assure you that seeking treatment for brain/mental health and learning problems is not a sign of weakness; it is a sign of strength and love for your child.COMMON CHILDHOOD MENTAL HEALTH ISSUES IN KIDS
Some of the more common mental health issues seen in children include:- ADD/ADHD: ADD/ADHD is characterized by a short attention span, distractibility, procrastination, disorganization, and poor internal supervision (such as problems with judgment and impulse control). Notice that hyperactivity is not one of the five hallmark symptoms.
- Anxiety disorders: All kids feel anxious from time to time. When anxiety becomes nearly constant, however, it may be an anxiety disorder.
- Depressive disorder: All kids feel sad or hopeless at times. But when low mood persists for weeks or months, it could be a sign of depression.
- Obsessive-Compulsive Disorder: OCD is characterized by unwanted, unpleasant recurrent thoughts that cause worry, shame, guilt, and/or compulsions that interfere with daily life. The most common repetitive behaviors involve counting, handwashing, checking, and touching.
- PANS and PANDAS: Pediatric autoimmune neuropsychiatric disorders associated with streptococcal infections (PANDAS), which are considered a subset of pediatric acute-onset neuropsychiatric syndrome (PANS), are mental and behavioral issues that occur suddenly following an infection.
RAISING MENTALLY STRONG KIDS
You will find the warning signs associated with these common childhood mental disorders, as well as natural solutions, in the book Raising Mentally Strong Kids. In the book, Raising Mentally Strong Kids, brain and mental health expert Dr. Daniel Amen and child psychologist Dr. Charles Fay have teamed up to reveal what’s missing from most parenting books. It’s the fact that you need to address both the brain and the mind of your child (and yourself) in order to be an effective parent and raise competent humans. In this groundbreaking, science-backed book where neuroscience meets practical psychology, parents are given proven tools to help children of all ages go from defiance, meltdowns, and power struggles to being responsible, resilient, and confident. Order your copy now and put your child on the path to a brighter future. If you want to join the tens of thousands of parents and children who have already learned how to be mentally stronger at Amen Clinics, speak to a specialist today at 888-288-9834 or visit our contact page here. Have you or a loved one ever experienced mental health symptoms or personality changes that seemed to have no definable source? If so, it might be helpful to get tested for Lyme disease. Lyme disease is transmitted by a tiny creature, the tick, but it can have an outsized array of negative impacts on physical and mental health. It can also trigger—or be misdiagnosed as—a wide variety of other conditions, and it’s often overlooked by medical professionals. This is especially devastating when someone undergoes drastic personality changes, with chronic Lyme disease as the unknown culprit. Personality changes can occur because this neuropsychiatric condition can impact moods, attention, and memory, or stir up feelings of anger or anxiousness. It may be mistaken for disorders such as borderline personality disorder (BPD) or lead to irritability or even violence, a phenomenon sometimes called Lyme rage. Let’s take a look at how and why Lyme disease can affect the personality, mimic various physical and mental health conditions, and lead to serious, even deadly, side effects. Lyme disease can affect the personality, mimic various physical and mental health conditions, and lead to serious, even deadly, side effects.LYME DISEASE SYMPTOMS
Lyme disease is a type of vector-borne disease, which means that it’s transmitted from animals to other animals (including humans). Lyme is spread when infected deer ticks pass along a bacteria named Borrelia burgdorferi. These eight-legged arachnids, also called black-legged ticks, attach to a host—often unnoticed, since they can be as small as poppy seeds—and feed on its blood. The bacteria can infect the host within just 36 to 48 hours, but the bacteria can lie dormant for months, or even years, in the central nervous system. If tick-borne disease symptoms do arise, their timetable varies—they can occur from 3 days to 30 or more days after the initial bite. The host may experience flu-like symptoms, the telltale bulls-eye rash, or swollen lymph nodes. But it’s also possible that no symptoms are apparent at all. A lack of symptoms can be dangerous because, without treatment, more serious side effects can develop. These can include facial palsy, limb and nerve pain, irregular heartbeat, joint pain and swelling, and gastrointestinal disturbances. In serious cases, inflammation of the brain and spinal cord can affect the central nervous system. These symptoms can mystify patients and doctors alike, since they can emulate those of other neurological disorders. For example, people may confuse Lyme with conditions such as fibromyalgia, dementia, traumatic brain injury, and chronic fatigue syndrome.HOW LYME DISEASE IMPACTS MENTAL HEALTH
Lyme affects the brain and the immune system, leading to inflammation. Evaluating the SPECT brain scans of patients with infectious diseases like Lyme, the brain looks as if it has been exposed to toxins. These changes can provoke detrimental effects on the personality, including symptoms like irritability or explosive anger, sometimes called Lyme rage. Both patients and loved ones have reported personality changes as a result of chronic Lyme disease. This may lead to symptoms associated with mental health conditions like borderline personality disorder, narcissistic personality disorder, schizoaffective personality disorder, and obsessive-compulsive disorder (OCD). Lyme disease may also mimic other psychiatric conditions, including psychotic disorders (such as delusions, paranoia, and schizophrenia), depression, anxiety disorders, and bipolar disorder. Given these damaging effects, it’s not surprising that Lyme disease is also associated with increased suicidality. A Danish study published in 2021 concluded that those diagnosed with Lyme displayed an increased risk of mental disorders, affective disorders, suicide attempts, and completed suicides. Lyme patients “had a 28% percent higher rate of mental disorders and were twice as likely to have attempted suicide post-infection, compared to individuals without the diagnosis,” according to a post-study report from the Columbia University Department of Psychiatry. Brian Fallon, MD, MPH, the lead author of the study, noted that Lyme disease is not only associated with a higher risk for severe cardiac, rheumatologic, and neurologic problems, but severe mental health problems as well. These findings backed up an earlier study that found links between suicidality and Lyme disease. Researchers hypothesized that immune-mediated and metabolic changes were the catalysts for psychiatric symptoms, which may be further aggravated by prevailing negative attitudes about Lyme. They added that some of these suicides “are associated with being overwhelmed by multiple debilitating symptoms, and others are impulsive, bizarre, and unpredictable.” Chronic Lyme disease creates additional far-reaching health impacts, according to another 2021 study that evaluated neuropsychiatric and psychological symptoms in 252 patients. It concluded that they experienced significantly lower quality of life and sleep, as well as cognitive impairments in the areas of attention and memory. Lyme patients also tended to have depressive symptoms. Only 3.1% of the patients were satisfied with their lives, while more than one-third of them (37%) scored in the lower third of the quality-of-life scale.DELAYED DIAGNOSIS AND MISDIAGNOSIS OF LYME DISEASE
The 252-patient study referenced above noted that, on average, patients didn’t get diagnosed with Lyme until they had visited almost 8 different physicians. That equated to 8 years passing between the initial tick bite and an official diagnosis. Overall, less than half of the patients (46%) received their diagnosis within the first 5 years after the onset of symptoms. In other words, Lyme disease is often diagnosed far too late. Difficulty diagnosing Lyme disease occurs for many reasons:- Blood tests for detecting Lyme disease early can be unreliable, since antibodies might not develop until weeks after the infection.
- Due to ticks’ small size, patients may not know they have been bitten—and there may be no obvious symptoms.
- Because the Borrelia burgdorferi bacteria can affect the brain, symptoms may mimic other disorders. Lyme has been called “the great imitator” for its tendency to be mistaken for other conditions.
- Borrelia burgdorferi bacteria can become dormant for months or years in the central nervous system.
- The Lyme pathogen type, known as a spirochete, can embed itself in cell membranes, including those in the brain, making it more difficult to detect.
- Symptoms can manifest long after a tick bite, so doctors as well as patients might overlook Lyme as a potential culprit.
THE DISTURBING STATISTICS ABOUT ADHD AND ADDICTIONS
Decades of research show that individuals with attention-deficit/hyperactivity disorder (ADHD), also called attention-deficit disorder (ADD), are more likely to develop substance use disorders than those without the mental health disorder. For example, adults with ADD/ADHD are about three times more likely to struggle with a substance use disorder (SUD) than their peers. Similarly, compared to kids who don’t have ADD/ADHD, children with the condition are two to three times more likely to abuse substances, according to a study in Clinical Psychology Review. In particular, research shows that children with ADD/ADHD are:- More than twice as likely to use nicotine
- Almost twice as likely to develop a dependence on alcohol
- Almost three times as likely to use marijuana and 1.5 times more likely to develop a cannabis dependence
- Twice as likely to develop cocaine dependence
ADHD AND THE BRAIN
ADD/ADHD is a brain-based disorder. The brain-imaging work using SPECT at Amen Clinics shows that the brain functions differently in people with this condition. Specifically, SPECT scans show abnormal activity in a part of the brain called the prefrontal cortex (PFC). This brain region is responsible for executive functions, such as planning, judgment, forethought, impulse control, and follow-through. In the healthy brain, concentration stimulates activity in the PFC. Not so in the ADD/ADHD brain. In people with this disorder, there’s a reduction in activity in the PFC when they try to concentrate. Effectively, this makes it harder for them to pay attention. The decreased activity in the PFC also helps explain the symptoms associated with the disorder. Brain imaging shows that having ADD/ADHD symptoms is not due to a lack of willpower or failing to try hard enough. Rather it’s related to the way the brain functions.ADHD AND THE BRAIN’S SELF-CONTROL CIRCUIT
ADD/ADHD is also associated with other brain functions, such as the self-control circuit. This circuit involves the brain systems that drive you to seek out things that bring you pleasure and the prefrontal cortex (PFC), which puts on the brakes when you are about to engage in risky behavior. In a healthy self-control circuit, an effective PFC provides impulse control and good judgment while the deep limbic system offers an adequate dose of motivation so you can plan and follow through on your goals. You can say no to alcohol, marijuana, cocaine, cigarettes, and other substances. When activity in the PFC is decreased, the drive circuits take control and cause you to lose control over your behavior. When this is the case, you’re more likely to fall victim to your cravings. Having low activity often results in a tendency for impulse-control problems and poor internal supervision. These contribute to the increased risk of addiction.SELF-MEDICATION AND THE ADHD BRAIN
Many people with ADD/ADHD self-medicate with substances in order to feel better—more focused, less anxious, less depressed, or less overwhelmed. Because the PFC is underactive in the ADD/ADHD brain, it can lead people to use substances as a way to stimulate brain activity. And those with hyperactivity may turn to other substances to calm down. Although these individuals abuse substances as a way to treat their underlying problems, it is bad medicine. Over time, substance abuse often exacerbates ADD/ADHD symptoms. The brain-imaging work at Amen Clinics clearly shows that substance abuse is harmful to brain function. Alcohol, marijuana, nicotine, cocaine, methamphetamines, and even caffeine reduce brain activity over time. In some cases, the reduction in brain activity can be significant. This means that when a teen with ADD/ADHD drinks alcohol to calm internal feelings of restlessness, it soothes them but only temporarily. At the same time, it damages cellular activity, which can lead to a worsening of symptoms in the long run. One study out of UCLA found that cocaine addicts had 23% less overall brain activity compared to individuals who had never taken drugs. In this study, the people addicted to cocaine who also smoked cigarettes had 45% less activity in their brain. Based on the clinical experience at Amen Clinics, people tend to use different substances based on which type of ADD/ADHD they have. The SPECT scans at Amen Clinics have helped identify 7 types of ADD/ADHD. People with Classic or Inattentive ADD/ADHD tend to use stimulants, such as cocaine or methamphetamine. Individuals with Overfocused ADD/ADHD are more likely to abuse alcohol. Having Temporal Lobe or Limbic ADD/ADHD makes people more inclined to use marijuana or stimulants. People with Anxious or Ring of Fire ADD/ADHD tend to abuse alcohol and marijuana.ADHD STIMULANT TREATMENT AND ADDICTION
Substance abuse often complicates the treatment of ADD/ADHD. As mentioned earlier, as many as 50% of adolescents and adults with ADD/ADHD also have substance abuse issues. Some people fear that stimulant medications may be a gateway drug to other substances. However, research has found that this is not the case. In fact, a 2016 study found that people who are taking prescription stimulants for ADD/ADHD are 7.3% less likely to develop a substance use disorder. However, many health care providers feel uncomfortable prescribing stimulant medications such as Ritalin or Adderall to people who have a substance use disorder. Physicians have to be very careful when this is the case. If you have an active addiction, you may need to wait until you’re enrolled in an addiction treatment program before a physician will prescribe stimulant medication for ADHD. After showing a sustained commitment to sobriety, you may be prescribed ADD/ADHD stimulants. Be aware that you will likely need to be monitored frequently. If you have ADD/ADHD, several lifestyle changes can also help prevent substance abuse. A healthy diet, daily exercise, and meditation are all natural ways to boost activity in the PFC to help you regain control. ADD/ADHD, addictions, and other mental health issues can’t wait. At Amen Clinics, we’re here for you. We offer in-clinic brain scanning and appointments, as well as mental telehealth, clinical evaluations, and therapy for adults, teens, children, and couples. Find out more by speaking to a specialist today at 888-288-9834 or visit our contact page here Divorce is a painful, stressful, and oftentimes traumatic event in the lives of those affected by it. When two people divorce, it commonly leads to anxiety and depression not only for the spouses but also for any children involved. Many people reach out to friends and family to help them work through the pain and learn to live with what has happened. Some seek help from a mental health therapist. This is a normal part of the grieving and recovery process. For some individuals, however, the trauma that they have endured from their divorce reaches so deep it can’t be healed through talk therapy alone. In some cases, it can lead to post-traumatic stress disorder (PTSD). For some individuals, the trauma that they have endured from their divorce reaches so deep it can’t be healed through talk therapy alone. In some cases, it can lead to post-traumatic stress disorder (PTSD).WHEN THE PAIN OF DIVORCE PERSISTS
Talk therapy isn’t always enough to help a person heal from the emotional trauma of divorce. This was the case for Jane, a 56-year-old woman who had divorced from her husband 18 years earlier. Even though she had seen more than one mental health counselor, she was still suffering from the wounds of her divorce. It felt as if no time had passed at all. “I had been suffering from a lot of anxiety, depression, and nagging, repetitive thoughts since then,” said Jane when she visited Amen Clinics for a more complete evaluation. “Those old tapes played over and over in my head.” Jane had seen multiple mental health therapists over the years, trying to get to the root of why she couldn’t move past the pain of her divorce nearly two decades later. She felt stuck in life, unable to move forward with her life even though she desperately wanted to heal. Jane had already tried talk therapy as well as emotion focused therapy (EFT)—also called emotionally focused therapy—without getting the results she wanted. “If they had told me that to feel better, I should stand on my head and spin around,” Jane said, “I would have given that a try as well!”HOW DIVORCE CAN LEAD TO PTSD
Finally, one of Jane’s therapists recommended looking at her pain through a new lens and suggested that she might have PTSD. Most people think that PTSD only occurs to military veterans who have seen combat, but that’s not the case. There are many nonviolent causes of PTSD. PTSD is associated with severe anxiety following a traumatic event, although it is not considered an anxiety disorder, according to experts. PTSD symptoms may include flashbacks, nightmares, avoidance of reminders of the trauma, emotional numbness, insomnia, and, in Jane’s case, uncontrollable thoughts about the event. PTSD can be a complex and sometimes confusing disorder. While two people may experience the same exact trauma, it isn’t a guarantee that both will later suffer from PTSD. Certain risk factors such as adverse childhood experiences (ACEs), past trauma, and a family history of clinical depression may make a person more susceptible to the disorder. As soon as Jane’s therapist suggested that she might have PTSD, she immediately began researching the disorder on her own. Most people affected with PTSD spend years trying to come to terms with the traumatic event that happened to them. “I consider myself a lifelong learner (meaning I read a lot) and so after coming across Dr. Amen on my local PBS channel, I ordered his books and read them all,” said Jane. “They made a lot of sense, so I investigated his clinics and what could be done for PTSD.” That’s when Jane decided to contact Amen Clinics and schedule an appointment. Jane’s comprehensive evaluation included a deep dive into the biological, psychological, social, and spiritual aspects of her life. She also took a sophisticated neuropsychological test that assesses cognitive, emotional, and intellectual functioning. In addition, she underwent a brain SPECT scan. This functional brain-imaging technology measures blood flow and activity in the brain. It shows areas of the brain with healthy activity, as well as areas that are either working too hard or not hard enough. Like most people with PTSD, Jane’s SPECT scan showed overactivity in several brain regions, including the following:- Deep limbic area
- Basal ganglia
- Anterior cingulate gyrus
NEUROFEEDBACK THERAPY FOR PTSD TREATMENT
As part of a personalized treatment program, Jane began neurofeedback therapy sessions and quickly began to feel relief. Neurofeedback is a non-invasive treatment that provides moment-to-moment feedback on physiological functioning. Several scientific studies have found that neurofeedback is beneficial for PTSD. Some research suggests that certain forms of neurofeedback should be part of standard treatment for trauma survivors. It focuses specifically on the central nervous system and the brain. This means that while the patient is experiencing an emotion, feedback is given about their physical systems such as heart and respiratory rates. This connection is then used to teach the patient about control while at the same time fostering a better understanding of the impact of their emotions on their physical selves. “I could notice gradual changes in my racing thoughts and depression,” said Jane. “But the real winning component in doing feedback is that I became anxiety-free.” Jane, who is now in recovery from PTSD, said it best, “It is such a gift to be free from all of those symptoms and to be relaxed and looking forward to life.” If you’re suffering from emotional trauma related to a divorce or breakup, it may be worth investigating if neurofeedback can help you regain emotional well-being. PTSD, anxiety, depression, and other mental health issues can’t wait. At Amen Clinics, we’re here for you. We offer in-clinic brain scanning and appointments, as well as mental telehealth, clinical evaluations, and therapy for adults, teens, children, and couples. Find out more by speaking to a specialist today at 888-288-9834 or visit our contact page here.This blog has been updated since it’s original publish date.
Do you find yourself forgetting your keys? Spacing out on why you walked into a room? Losing your train of thought mid-sentence? If you answered yes to any of these questions and you’re also a couch potato, there is one important strategy that could put you on the path to improved recall.
The secret to a better memory? Moving more.
Aerobic exercise provides greater blood flow to your brain, especially to the hippocampus, a region that’s crucial to memory. A 2017 study in 51 healthy men and women, ages 18-35, found that those who had the highest fitness levels had a firmer, more elastic hippocampus and scored the best on memory tests.
Research shows that reduced blood flow is the #1 brain-imaging predictor that a person will develop Alzheimer’s disease.BLOOD FLOW AND THE BRAIN
Healthy blood flow is crucial to your brain—and to your whole body. It transports nutrients, including oxygen, to every cell in your body and flushes away toxins. Even though your brain, which weighs about 3 pounds, makes up only 2% of your body’s weight, it uses 20% of the oxygen and blood flow in your body.
Exciting new research in Human Brain Mapping dispels the long-held belief that our brain cells age quickly; rather, it is the blood vessels that feed our neurons that are aging faster. If you want to keep your brain healthy, your mind sharp, and your mental health strong for as long as possible, you need to protect your blood vessels.
If you keep your blood vessels healthy, you may be able to avoid not only memory loss and Alzheimer’s disease, but also a host of mental health issues (see below) as well as physical problems like high blood pressure, heart disease, stroke, and erectile dysfunction, among others. You’ll also have a lot more energy and you’re less likely to be overweight.
BRAIN HEALTH PROBLEMS OF LOW BLOOD FLOW
Anything that damages your blood vessels or impairs blood flow hurts your brain. Brain SPECT imaging studies reveal that low blood flow is related to many behavioral and psychiatric issues. SPECT is a type of brain imaging study that measures the brain’s blood flow and activity. Low blood flow seen on SPECT has been seen with:
- Memory loss and Alzheimer’s disease
- Depression
- Suicide
- Bipolar disorder
- Schizophrenia
- ADD/ADHD
- Traumatic brain injury
- Hoarding
- Murder
- Substance abuse
In fact, research in Nature Communications shows that low blood flow is the #1 brain imaging predictor that a person will develop Alzheimer’s disease.
11 WAYS EXERCISE PROTECTS MEMORY
Here are some of the many ways physical exercise enhances brain health and protects memory:
- Helps increase the size of the hippocampus, the Holy Grail of any memory enhancement program, according to the American Journal of Geriatric Psychiatry and several other studies.
- Protects the hippocampus from stress-related hormones, like cortisol, which normally shrinks it. Even leisurely walking has been shown to increase the size of the hippocampus in women, according to findings in Hippocampus.
- Stimulates the production of growth factors, such as BDNF (brain-derived neurotrophic factors), which nurture stem cell production.
- Stimulates “neurogenesis,” the ability of the brain to generate new neurons
- Decreases the formation of beta-amyloid plaque, clumps of protein found in the brains of people with Alzheimer’s disease, according to the Journal of Neuroscience.
- Improves cognitive flexibility, as shown in 2015 research in Current Biology.
- Improves mood, which is important because research shows depression has been linked to an increased risk of developing Alzheimer’s disease.
- Enhances insulin’s ability to lower high blood sugar levels, reducing the risk of diabetes. In some scientific journals, Alzheimer’s has been called “type 3 diabetes.”
- Allows for greater detoxification through sweat, which is critical because toxins in any form damage the brain and increase the risk of memory problems and dementia.
- Improves the quality of sleep. Some scientific research suggests that sleep disturbances may be a predictor of Alzheimer’s.
- Improves immunity. Several studies have found immune system dysfunction in dementia.
WHICH EXERCISES ARE BEST FOR YOUR BRAIN?
Racquet sports are particularly beneficial. A 2016 study in the British Journal of Sports Medicine that followed more than 80,000 adults found that those who played tennis, table tennis, squash and other racquet sports had the lowest risk of dying during the nearly decade-long research. Swimming and aerobics are good choices, too. And if you walk, just be sure to keep up the pace to get the most benefits.
MORE WAYS TO BOOST BLOOD FLOW
In addition to physical exercise, there are many other ways to improve your blood flow, including treating high blood pressure, cholesterol, or other vascular problems, and avoiding cigarettes and caffeine, which constrict blood flow to the brain. Here are more easy, beneficial moves:
- Hydrate better! Drinking at least 5 glasses of water a day could decrease your risk of hypertension
- Drink more green tea
- Limit salt intake
- Take a good multivitamin/mineral, vitamin D, magnesium and an omega-3 EPA/DHA supplement daily
- Support your memory with ginkgo biloba extract
- Enjoy an ounce of dark chocolate every day (for the cocoa flavanols)
- Eat more beets, green leafy vegetables, berries, pumpkin seeds, and cayenne pepper
- Increase your intake of foods high in magnesium, such as avocados, nuts, and seeds
- Eat more foods loaded with potassium, such as spinach and sweet potatoes
- Limit alcohol, fruit juices, and sodas (including diet sodas)
- Sleep 7 to 8 hours a night, and if you have sleep apnea, get it assessed and treated
- Try hyperbaric oxygen therapy (HBOT), a simple, non-invasive, painless treatment with minimal side effects that use the power of oxygen to enhance the healing process. Before-and-after SPECT scans of people who have undergone HBOT reveal remarkable improvement in blood flow.
Blood flow is so important, it is the first risk factor in the Amen Clinics Memory Rescue BRIGHT MINDS Program, which identifies and treats the 11 risk factors that can steal your memory and your mind. Preventing and treating these risk factors is the best way to keep your memory sharp for the rest of your life.
We are available for in-clinic brain scanning and appointments, as well as mental telehealth, remote clinical evaluations, and video therapy. Find out more by speaking to a specialist today at 888-288-9834. If all our specialists are busy helping others, you can also schedule a time to talk.
Are you finding it harder to pay attention these days? You’re not alone. A study by Microsoft found that the human attention span has dwindled to just 8 seconds. That’s less than the 9-second attention span of a goldfish! In part, you can blame our fast-paced, digital society for the dramatic decrease. With our phones, laptops, tablets, and digital personal assistants pinging and buzzing constantly, it’s nearly impossible not to get distracted. That’s bad news for anyone who wants to succeed in life. Whether you’re working on a big project at work, developing a new product line for your business, or taking a professional course, concentration is key. What can you do to regain your mental focus in the face of distractions? The first step is optimizing your brain, especially a region called the prefrontal cortex that’s heavily involved in focus, planning, and follow-through. With our phones, laptops, tablets, and digital personal assistants pinging and buzzing constantly, it’s nearly impossible not to get distracted. That’s bad news for anyone who wants to succeed in life.WHAT IS THE PREFRONTAL CORTEX?
The prefrontal cortex (PFC) is the most evolved part of the brain. As such, it is essential in helping you reach your goals. The PFC is responsible for executive functions, which are higher-level cognitive skills. These brain functions include concentration, attention span, judgment, impulse control, organization, follow-through, empathy, and critical thinking. This brain region controls your ability to look at situations, organize your thoughts, plan what you want to do, and carry out your plans. When the PFC is healthy, it makes it easier for you to carry out these functions. When your prefrontal cortex is low in activity, it’s more challenging. Functional brain imaging with a technology called SPECT proves it. At Amen Clinics, which has built the world’s largest database of SPECT scans, the images from tens of thousands of patients show that blood flow and activity in the prefrontal cortex are critical for focus. Low blood flow and activity in the PFC are associated with difficulty concentrating, poor impulse control, disorganization, poor judgment and more. It is also a common sign of attention-deficit/hyperactivity disorder (ADHD), also called attention-deficit disorder (ADD). People with ADD/ADHD also have lower levels of the neurotransmitter dopamine. This is linked to decreased motivation and focus. The good news is that you can boost activity in the PFC and improve focus and attention with some simple lifestyle changes. Here are 5 neuroscience-based tips to enhance prefrontal cortex function to help you have better focus.5 LIFESTYLE STRATEGIES FOR BETTER FOCUS
- Eat a diet that’s higher in protein.
- Listen to classical music.
- Meditate or pray daily.
- Focus on what you love.
- Do your best to stay organized.
STAY FOCUSED ON YOUR ABILITY TO PAY ATTENTION
Focus and attention are so important in life. Make it a priority to keep an eye on your ability to concentrate. By implementing the strategies in this blog, you’ll be better able to stay on track to reach your goals. If you find that after putting these tips into action, you’re still struggling, seek help from a mental health professional. Be sure to look for a provider who understands that the brain’s prefrontal cortex is the key to improving focus and attention and who provides brain-based treatment plans. ADD/ADHD and other mental health issues can’t wait. At Amen Clinics, we’re here for you. We offer in-clinic brain scanning and appointments, as well as mental telehealth, clinical evaluations, and therapy for adults, teens, children, and couples. Find out more by speaking to a specialist today at 888-288-9834 or visit our contact page here. This post has been updated from it’s original publish date. If you have ADHD, also called ADD—or if you have a child with ADHD—it can make life more challenging in so many ways. For example, people may think you’re lazy because you show up late for work, or because you wait until the last minute to start your household chores or work assignments. Your child may impulsively say rude things, which makes it hard for them to make friends. And that can have a negative effect on the trajectory of their life. It can make them feel like a failure. What you may not realize is that attention-deficit/hyperactivity disorder (ADHD), or attention-deficit disorder (ADD), isn’t your fault. It’s due to faulty brain activity in an area called the prefrontal cortex. Learning more about this important brain region and how it functions in people with the mental health disorder can change the way you view yourself or your child. And it can lead the way to better control over ADD/ADHD symptoms. What you may not realize is that ADD/ADHD isn’t your fault. It’s due to faulty brain activity in an area called the prefrontal cortex.WHAT IS THE PREFRONTAL CORTEX?
The prefrontal cortex (PFC), also known as the brain’s “executive center,” is the most evolved part of the brain. It occupies the front third of the brain, behind the forehead. It is often divided into three sections: • Dorsal lateral section—on the outside surface of the PFC • Inferior orbital section—on the front undersurface of the brain • Anterior cingulate gyrus—which runs through the middle of the frontal lobes The PFC is involved in many functions, such as: • Focus and attention • Planning • Organization • Forethought • Judgment • Empathy • Impulse control • Learning from mistakes • Follow-through Healthy PFC activity helps people think through the consequences of their behavior, which is essential for effective living in nearly every aspect of life. It impacts decisions related to: • Choosing a good mate • Interacting with customers • Dealing with difficult children • Spending money wisely • Driving safely on the freeway Without proper PFC function, it’s difficult to act in consistent, thoughtful ways, and impulses can take over. Damage to the prefrontal cortex can have far-reaching effects, such as with YouTube star Logan Paul. The YouTuber’s decision-making often lands him in hot water and made him the most hated celebrity in 2018.ADD/ADHD IS A BRAIN-BASED DISORDER
ADD/ADHD is a neurodevelopmental disorder. Functional brain imaging with SPECT scans shows that it is associated with abnormal function in the prefrontal cortex. On SPECT scans of people with healthy brain function, the act of concentrating increases activity in the PFC. However, when those with ADD/ADHD try to concentrate, PFC activity decreases rather than increases. Healthy Brain SPECT Scan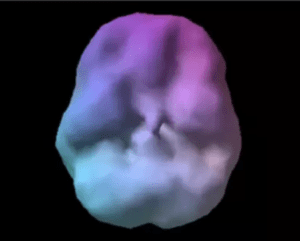
In the healthy brain, there is full, even, symmetrical blood flow/activity.
ADD/ADHD Brain SPECT Scan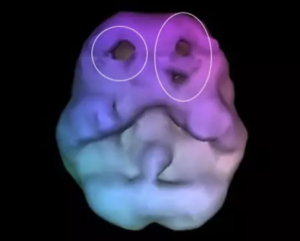 In the ADD/ADHD brain, there is low blood flow/activity in the prefrontal cortex. In the image here, the holes indicate areas of low blood flow.
Due to low activity in the PFC, people can struggle with a range of ADD/ADHD symptoms, such as:
In the ADD/ADHD brain, there is low blood flow/activity in the prefrontal cortex. In the image here, the holes indicate areas of low blood flow.
Due to low activity in the PFC, people can struggle with a range of ADD/ADHD symptoms, such as:
- Poor internal supervision
- Short attention span
- Distractibility
- Disorganization
- Hyperactivity (although only half the people with ADD are hyperactive)
- Impulse control problems
- Difficulty learning from past errors
- Lack of forethought
- Procrastination
ADD/ADHD AND THE PREFRONTAL CORTEX
Here are some common characteristics of ADD/ADHD that clearly connect this disorder to the PFC:-
The harder you try, the worse it gets.
-
You have difficulty paying attention.
-
You get easily distracted.
-
You say and do things impulsively.
-
You like drama.
SUPPORT THE PREFRONTAL CORTEX
Anyone with ADD/ADHD needs to support the brain for better prefrontal cortex function. Strategies to optimize the PFC include:- Neurofeedback: Studies show that neurofeedback treatment improves ADD/ADHD symptoms.
- Goal setting: Knowing what you want out of life can help you match your behavior to achieve your goals.
- Meditation: Studies show that meditation enhances function in the PFC.
- Higher-protein diet: Eating a diet that is higher in protein and lower in simple carbohydrates improves focus.
- Nutraceuticals: Take supplements, such as omega-3 fatty acids, rhodiola, green tea extract, zinc, ginseng, and ashwagandha.
5 Tips for Reaching the Underachieving Child
Excerpted from Raising Mentally Strong Kids, by Daniel Amen, MD, and Charles Fay, PhD Underachievement is one of the most complex challenges facing children, parents, and schools, and it can have devastating effects on a young person’s sense of self-worth and mental strength. Too often, parents start with the assumption that the child is simply being lazy. Then these well-meaning adults often resort to practices that make the problem worse. Here’s an overview of methods that seem like they should work but that tend to backfire. Plus, you’ll find 5 proven tips for reaching the underachieving child to boost their confidence, motivation, and performance. Underachievement is one of the most complex challenges facing children, parents, and schools, and it can have devastating effects on a young person’s sense of self-worth and mental strength.WORST WAYS TO MOTIVATE UNDERACHIEVING KIDS
Some of the most common but wrong ways to try to motivate underachieving children include:- Threats
- Lectures
- Reminders
- Punishment
- An excessive focus on remediating weaknesses at the expense of nurturing strengths
- Providing consequences that restrict the child from healthy social and physical activities
- Resentment
- Dependency
- Entitlement
- Anxiety
- Hopelessness
5 TIPS FOR RAISING AN ACADEMICALLY SECURE AND MOTIVATED CHILD
Tip #1: End the control battle.
As soon as a control battle begins, anxiety increases and academic motivation decreases. As soon as power struggles start, the bond we have with our kids weakens. Control battles can damage many aspects of our children’s development.Tip #2: Transition responsibility for learning to your child.
Whose learning are we talking about? Is it yours or your child’s? Obviously, you can’t do school for your kids. While true, this doesn’t stop many parents from taking way more ownership in their kids’ learning than their kids do.Tip #3: Respond with empathy and reasonable, logical consequences.
Anger shuts the door on learning. Empathy opens the door to learning. Anger implies that the problem is ours. Empathy allows it to remain our child’s. Empathy, in and of itself, assists in meeting most of the needs for love and belonging. It calms anxiety, and it helps us communicate that we understand our child’s feelings.Tip #4: Follow some guidelines for helping with homework.
Successful parents care about their children’s homework, and they follow some basic guidelines for helping in productive ways:- Help as long as your child wants it from you.
- Help only when your child can prove that they listen to their teacher.
- Help only as long as there is no anger or frustration.
- Help in brief segments, so that they can see themselves succeeding.
