

Bipolar Disorder
Bipolar disorder is a serious mood disorder that is frequently misdiagnosed. Amen Clinics goes beyond traditional mental health care by using brain imaging to identify the root cause of your symptoms for more targeted and effective treatment.
What Is BIPOLAR DISORDER?
Bipolar disorder, previously known as manic-depressive illness, is a brain disorder that results in significant and severe changes in mood, energy, activity levels and ability to carry out routine tasks. These shifts are more severe than the normal ups and downs that most people experience. According to the World Economic Forum, bipolar disorder ranks sixth on the list of the world’s leading causes of disability.
Who has Bipolar Disorder?
Nearly 6 million adults in America are affected by bipolar disorder, which can also affect children and adolescents. The onset of the disorder most commonly begins in young adulthood (late teens to mid-20s), but it can also start in childhood or as late as in a person’s 50s.
Men and women are equally likely to develop the disorder, which tends to run in families. People with a parent or sibling with the condition are more likely to develop it. This indicates there may be a genetic factor involved. However, it’s important to know that having a family member with the condition does not mean that you will get it too. In addition, remember that your genetics are not your destiny. A growing body of evidence shows that your lifestyle habits can either turn on or turn off your genes.

What are the Core Symptoms?
Because bipolar disorder involves both manic episodes and depressive episodes that shift in a cyclical pattern, people with the condition typically experience a broad range of symptoms. Manic episodes are characterized by many things, including decreased need for sleep, grandiose ideas, or racing thoughts. Depressive episodes are characterized by loss of interest in usually pleasurable activities to even thoughts of death or suicide. See below for more details about these two types of episodes.

Untreated BIPOLAR DISORDER CAN CAUSE MAJOR PROBLEMS IN LIFE
- Relationship problems
- Poor school performance
- Difficulty with occupational functioning
- Unemployment
- Legal and financial issues
- Substance abuse
- Chronic medical illnesses
- Potential life expectancy decrease of 10 to 12 years
- 20 – 30 times greater risk of suicide

What Causes BIPOLAR DISOrDER?
Experts have yet to discover the exact causes of bipolar disorder, but they have identified several risk factors for the condition. As you saw above, having one or more family members with bipolar disorder increases the risk. So does a history of emotional trauma, high stress, or substance abuse. In addition, bipolar disorder is associated with changes in the structure and function of the brain (see below for more on this).

Why Choose Amen Clinics for Treating Bipolar Disorder?
Bipolar disorder is often misdiagnosed as depression, ADD/ADHD, or even schizophrenia because some of the symptoms are very similar. Making the distinction between bipolar disorder and other conditions is critical because following the wrong treatment plan can make symptoms much worse. For example, when someone with bipolar disorder is misdiagnosed with ADD/ADHD and given stimulant medication, it can dramatically exacerbate symptoms and cycling. At Amen Clinics, we use brain imaging as part of a comprehensive evaluation to help distinguish between bipolar disorder, ADD/ADHD, depression, schizophrenia, and other conditions. This means you’ll get a more effective treatment plan.
BIPOLAR Brains Work Differently
In brain SPECT images of people with bipolar disorder, we see heightened activity in the limbic system which includes the amygdala, the hippocampus, and the cingulate gyrus. This system controls emotion, memory, motivation, fear, and sensory information. Abnormalities in this region can impact one’s emotional and sensory states negatively impacting their daily lives. By knowing which area of the brain is most impacted, we can customize a treatment plan and approach to calm areas of the brain working too hard and stimulate areas of the brain not working hard enough.
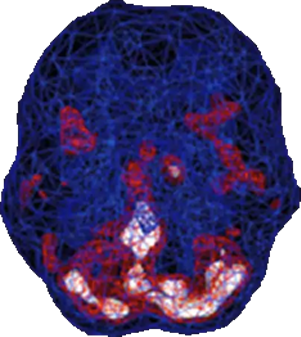
SPECT (single photon emission computed tomography) is a nuclear medicine study that evaluates blood flow and activity in the brain. Basically, it shows three things: healthy activity, too little activity, or too much activity. A healthy “active” scan shows the most active parts of the brain with blue representing the average activity and red (or sometimes red and white) representing the most active parts of the brain. In the healthy scan on the top right, the most active area is in the cerebellum, at the back/bottom part of the brain. In the scan below it from a person with bipolar disorder, there is overactivity in many areas of the brain.
Cyclic mood disorders, such as bipolar disorder, often correlate with focal areas of increased activity in the limbic system as well as too much activity across the surface of the brain. SPECT brain scans also show that many people who are diagnosed with bipolar disorder actually have a traumatic brain injury that has never been properly diagnosed and treated. For these people, healing the underlying TBI can be very helpful in alleviating symptoms associated with bipolar disorder.
Healthy Brain Scan
Bipolar Disorder Scan
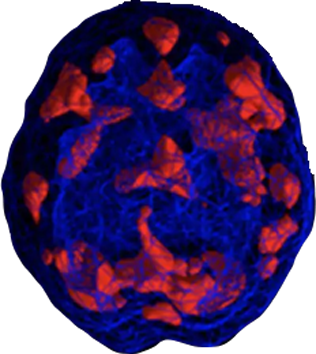
Bipolar Disorder features both manic episodes and depressive episodes that shift in a cyclical pattern. People with this condition typically experience a broad range of symptoms.
Types of BIPOLAR EPISODES
Manic Episodes
Manic episodes are characterized by an enduring emotional state that is expansive and elevated or irritable, and leads to unusually increased energy and activity.
Symptoms of mania include:
- Inflated self-esteem or sense of invincibility
- Grandiose notions, ideas, or plans
- Pronounced and abnormal elevation in mood
- Irritability or aggression
- Feeling agitated or euphoric
- Increased goal-directed activity, whether rational or not
- Notable decreased need for sleep that doesn’t diminish energy levels
- Increased talkativeness or rapid/pressured speech
- Racing thoughts and feeling “wired”
- Distractibility and restlessness
- Impulsivity
- Poor judgment that leads to risky and consequential behavior, such as unrestrained shopping sprees, unwise business endeavors, or promiscuity
- Inappropriate social behavior
- Delusions or hallucinations
- Suicidal thoughts or attempts, or dying by suicide
Bipolar I disorder is defined by having at least one episode of mania that lasts a week or longer and significantly disrupts occupational and social functioning. A person in a full-blown manic state may not be able to recognize that their symptoms are abnormal. In some cases, the impairment caused by mania can lead to the threat of harm to others or themselves, exhaustion, or psychosis—all of which might require inpatient hospitalization.
In bipolar II, elevated symptoms last at least four days, and while observable by others, they do not interfere with important areas of functioning; hence, the reason they are known as hypomanic episodes.
Depressive Episodes
Depressive episodes in bipolar disorder are marked by a significant—and sometimes severe—downshift in mood and energy that lasts at least 2 weeks, and causes serious symptoms that interfere with multiple areas of a person’s life.
Depressive symptoms include:
- Persistent sad or negative mood
- Loss of interest in usually enjoyable activities
- Feelings of guilt, worthlessness, helplessness, or hopelessness
- Insomnia, sleeping too much, or waking up too early
- Low energy, fatigue, or feeling “slowed down”
- Difficulty concentrating and making decisions
- Notable increase or decrease in appetite or weight
- Psychotic symptoms
- Thoughts of death, suicidal ideation, suicide attempts or completion
More than half of manic/hypomanic episodes occur right before a descent into depression. Those who have bipolar I disorder might have an episode of depression following mania or they may not get depressed and instead become euthymic, which is a more stable and tranquil mood state. The pattern for people who have bipolar II is hypomania that alternates with episodes of depression, although they may have intermittent periods of euthymia. It is also possible for a person to have mixed state episodes during which they experience both manic/hypomanic and depressive symptoms.
Cyclothymic Disorder
This condition, sometimes referred to as “cyclothymia,” is also a fluctuating mood condition but differs from bipolar I and II in a few ways. Someone with this disorder experiences a chronic pattern of fluctuating hypomanic and depressive symptoms, but they are considerably less severe than those seen in the bipolar disorders. As much as 2.5% of the U.S. population may struggle with this condition that can begin in childhood, but often starts in adolescence or early adulthood. There is up to a 50% chance that someone who has cyclothymia may eventually develop either of the bipolar disorders.


