ARCHIVE
In August, former First Lady Michelle Obama revealed on her podcast that “I am dealing with some form of low-grade depression.” She’s not the only one. Pandemic-related depression is sweeping across the nation and around the world. A survey in JAMA Network Open found that the rate of depression symptoms in the U.S. increased more than 3-fold during the COVID-19 pandemic, jumping from 8.5% before the pandemic to nearly 28%. But depression has also been linked to having COVID-19. A 2020 study in the Journal of Alzheimer’s Disease shows that one of the consequences of COVID-19 includes depression, in addition to anxiety, attention problems, obsessive compulsive disorder, memory loss, and more. Another 2020 study appearing in the journal Laryngoscope found that in people with COVID, experiencing a loss of smell and taste was associated with depressed mood and anxiety. New research shows that up to 80% of people with COVID report experiencing anosmia, or the loss of smell. Surprisingly, depression and anxiety were more likely to be found in people with olfactory dysfunction than in those with other symptoms, such as shortness of breath, fever, or cough.THE SCIENCE OF SMELL AND MOOD
A wealth of scientific research has shown that our sense of smell and our moods are intertwined. For example:- When scientists chemically blunted the sense of smell in mice for a 2018 study, it induced depressive behavior in the rodents.
- In another study on elderly Koreans, an impaired olfactory function was associated with a significantly higher degree of depression in addition to lower cognitive performance and decreased quality of life.
- A 2016 review of the existing research on anosmia and depression showed that the relationship appears to be a 2-way street. People with depression are more likely to have problems with a sense of smell than healthy controls, and people with anosmia are more likely to have symptoms of depression. And the greater the loss of smell the more severe the depressive symptoms.
SENSE OF SMELL AND EMOTIONS IN THE BRAIN
The area of your brain involved with smell (olfactory cortex) is located near your limbic system (the brain’s emotional centers), including the hippocampus, which is involved with mood and memory. These areas tend to deteriorate and die together. Not only is the loss of smell associated with depression, but it is also linked to memory loss and Alzheimer’s disease. Having trouble smelling peanut butter, lemon, strawberries, or natural gas is associated with a higher incidence of significant memory problems, according to research. Scoring poorly on a smell test is considered a warning sign of Alzheimer’s disease later in life. If you experience a diminishing sense of smell or the sudden loss of your ability to identify scents, it may be a sign of trouble. Take note of any other health symptoms (fever, cough, fatigue) that may be related to COVID-19, and take stock of your emotional well-being and memory to see if you notice any changes. Be sure to make an appointment with a healthcare professional.SMELL THE ROSES
To improve your sense of smell, give your sniffer a daily workout. There is evidence that repeated exposure to certain odors can improve the ability to smell. In a study from Aristotle University in Greece, 111 patients with anosmia repeatedly trained their sense of smell twice a day using 4 odors (phenyl ethyl alcohol, eucalyptol, citronellal, eugenol). After 8 weeks, compared to a control group, participants noticed significant improvement that lasted up to a year. If you have this issue, put your nose to work. Certain scents have also been found to improve mood and ease depression. Essential oils that support healthy moods include lavender, chamomile, rose oil, lemon, and jasmine. Depression, memory loss, and other mental health issues can’t wait. During these uncertain times, your mental well-being is more important than ever and waiting until life gets back to “normal” is likely to make your symptoms worsen over time. At Amen Clinics, we’re here for you. We offer in-clinic brain scanning and appointments, as well as mental telehealth, remote clinical evaluations, and video therapy for adults, children, and couples. Find out more by speaking to a specialist today at 888-288-9834. If all our specialists are busy helping others, you can also schedule a time to talk. Professional football players seem invincible, but beneath their imposing physical stature, they face the same mental health issues as the rest of us. In fact, considering the number of hits to the head and concussions they experience, they’re often at increased risk of anxiety, depression, ADD/ADHD, and more. Research shows that due to the stigma attached to mental health problems as well as other reasons, these sports superstars often choose to stay silent about their inner issues. Not Dak Prescott. The quarterback for the Dallas Cowboys recently spoke openly about his own struggles with anxiety and depression following his brother’s suicide, his mother’s battle with colon cancer, and the pandemic. On “In Depth with Graham Bensinger,” Prescott says, “I think that it’s important to be vulnerable, to be genuine, and to be transparent.” The QB says he got the help he needed, and it allowed him to get over his mental health issues. Not everybody in the NFL is so lucky. Take Aaron Hernandez, for example. Hernandez played for the New England Patriots and went from living the dream as an NFL player to being deeply troubled and convicted of murder. He eventually died by suicide at age 27.Studying the Brains of NFL Players
Amen Clinics has been treating professional football players and studying their brains for over a decade. In 2009, Amen Clinics performed the world’s first and largest brain imaging study on active and retired NFL players. Many of them complained of memory problems and scored very poorly on the cognitive tests. As a group, their brain SPECT scans looked awful. SPECT is a functional brain imaging technology that measures blood flow and activity in the brain. It shows areas that have healthy activity, too much activity, or not enough activity. The treatment arm of this study included brain health education and targeted nutraceuticals. The Amen Clinics protocol used in the study demonstrated increased blood flow to multiple brain areas, including the prefrontal cortex and hippocampus, and improvements in memory, attention, and processing speed. In a 2011 study by Amen Clinics on 100 active and former NFL players, the results were very clear: Playing football damaged multiple areas of the brain in greater than 90% of the players. There was persistent damage to the following areas of the brain:- Prefrontal cortex (judgment, planning, forethought, and impulse control)
- Temporal lobes (learning, memory, and mood stability)
- Cerebellum (mental agility and processing speed)
Head Trauma, Mental Well-Being, and Cognitive Health
You don’t have to be a professional football player to experience a traumatic brain injury (TBI) that impacts your mental and cognitive health. Playing tackle football at any level can put you at risk for head injuries. So does hitting soccer balls with your head, falling off a skateboard or bike, or getting hit in the head with a hockey puck or a baseball. Many head injuries are caused by everyday accidents like falling off a ladder, slipping in the shower, or being involved in a car accident. Brain SPECT imaging shows that head trauma is a major cause of psychiatric illness. However, very few people know it because most mental health professionals never look at the brains of their patients. A wealth of research shows that head injuries increase the risk of:- ADD/ADHD
- Aggression
- Anxiety
- Panic disorders
- Borderline and antisocial personality disorders
- Dementia
- Depression
- Drug and alcohol abuse
- Psychosis
- Post-traumatic stress disorder (PTSD)
- Suicide
- Learning problems
Help for Healing from Head Injuries
If you (or a loved one) have suffered a head injury, there is hope for healing. First, you have to fall in love with your brain and get serious about brain health. This includes good nutrition, regular exercise, adequate sleep, and avoiding exposure to toxic substances (including alcohol and drugs). In addition, here are some specific strategies for anyone who’s suffered a head injury.Protect your head from future injuries:
Experiencing multiple head injuries increases the risk of anxiety, depression, ADD/ADHD, memory loss, and other issues. If you’ve already experienced a TBI, it’s even more important to avoid another one.Check your hormone levels:
Blows to the head often damage the pituitary gland, which regulates your hormones, causing major hormonal imbalances that can cause symptoms related to depression, anxiety, brain fog, and more.Neurofeedback:
This non-invasive treatment may help you gain control of your brain waves through self-regulation. There are more than 1,000 studies showing that neurofeedback can help with TBI, depression, ADD/ADHD, obsessive compulsive disorder (OCD), addiction, memory in healthy people, and more.Hyperbaric oxygen therapy (HBOT):
HBOT is a simple, non-invasive, painless treatment that uses the power of oxygen to enhance the healing process and boost blood flow. Brain imaging studies using SPECT show that people who have had HBOT have marked improvement in blood flow to the brain. A 2013 study in Plos One on 56 mild TBI patients with post-concussion syndrome showed that HBOT improved cognitive and emotional functioning and quality of life. HBOT has been used to improve many issues, including TBI, anxiety and depression, post-traumatic stress disorder (PTSD), attention problems, memory problems, and more. NFL Hall-of Fame quarterback Joe Namath revealed that he used HBOT to help heal the damage to his brain from at least 5 concussions he had suffered. He had been concerned about the health of his brain and got a SPECT scan from a hospital in Florida, which revealed evidence of TBI. Head trauma, anxiety, depression, ADD/ADHD, and other mental health conditions—can’t wait. During these uncertain times, your mental well-being is more important than ever, and waiting until life gets back to “normal” is likely to make your symptoms worsen over time. At Amen Clinics, we’re here for you. We offer in-clinic brain scanning and appointments, as well as mental telehealth, remote clinical evaluations, and video therapy for adults, children, and couples. Find out more by speaking to a specialist today at 888-288-9834. If all our specialists are busy helping others, you can also schedule a time to talk. When superstar influencer Laura Clery got a brain scan as part of an evaluation at Amen Clinics, she received a diagnosis she never expected—ADD. “Even though I really struggled to focus growing up… and I struggled to take tests, and I never felt very smart,” she says in the Instagram TV post she shared with her 10 million social media followers, “I never really thought about [ADD].” The comedian says she thought she was just lazy and easily distracted as if it was a character flaw. When she was younger, Clery had been diagnosed with bipolar disorder, but that diagnosis didn’t fit. Clery isn’t alone. At Amen Clinics, the global leader in brain health, thousands of women who had been previously misdiagnosed have learned they actually have ADD (also known as ADHD). There are potentially hundreds of thousands or even millions of women across the U.S. who are struggling with undetected ADD. You may be one of them. And it could be impacting your self-esteem, career, relationships, and personal health and fitness. In the worst-case scenario, it could be ruining your life. Why do so many women with this common condition remain undiagnosed or misdiagnosed? Because ADD looks different in females than in males. Why do so many women with this common condition remain undiagnosed or misdiagnosed? Because ADD looks different in females than in males.ADD SYMPTOMS IN WOMEN
Most people think of ADD as a condition that is primarily seen in males who are hyperactive and impulsive. In fact, women are just as likely as men to have ADD, according to a 2016 paper in The ADHD Report. Even more surprising is the fact that women experience more severe ADD symptoms than their male counterparts, according to a study in the Journal of Clinical Psychiatry. However, women tend to have a different type of the condition that comes with its own set of symptoms. The brain imaging work at Amen Clinics, which has the world’s largest database of functional brain scans related to behavior, has helped identify 7 types of ADD. The type that is most common in females is called Inattentive ADD. Although it’s the second most common type of the condition, its symptoms often go unrecognized by many medical professionals. Unfortunately, many women with Inattentive ADD never get diagnosed. Instead, they’re labeled as slow, lazy, spacey, or unmotivated. Unfortunately, many women with Inattentive ADD never get diagnosed. Instead, they’re labeled as slow, lazy, spacey, or unmotivated. While people with Classic ADD, the most common type of the condition, bring negative attention to themselves with their hyperactivity, constant chatter, and conflict-driven behavior, women with Inattentive ADD tend to be quiet and distracted. Rather than cause problems, they’re more likely to daydream or look out the window. They’re not as likely to be impulsive or to blurt out inappropriate or hurtful things. They’re frequently thought of as couch potatoes who have trouble finding interest or motivation in their lives.Core symptoms of all types of ADD include:
- Easily distracted
- Short attention span
- Difficulty following through (procrastination) on tasks or instructions
- Difficulty keeping an organized area (room, office, desk, filing cabinet, car, etc.)
- Has trouble with time, for example, frequently late or hurried, tasks take longer than expected, projects are “last minute” or turned in late
- Forgetfulness
- Problems with follow-through
- Poor impulse control
Unique symptoms of Inattentive ADD include:
- Problems with focus
- Tendency to lose things
- Makes careless mistakes
- Poor attention to detail
- Forgetful
- Excessive daydreaming
- Complaints of being bored
- Apathy or lack of motivation
- Tired, sluggish, or slow-moving
- Seems spacey or preoccupied
CONSEQUENCES OF UNTREATED OR MISDIAGNOSED ADD IN WOMEN
Having undiagnosed or untreated ADD comes with a very high cost. And it increases the risk of many other issues, including:- Anxiety
- Depression
- Addiction
- Eating disorders
- Obesity
- Obsessive compulsive disorder (OCD)
- Post-traumatic stress disorder (PTSD)
- Sleep disorders
- Divorce
- Career problems
INATTENTIVE ADD IN THE FEMALE BRAIN
On her IGTV post, Clery shared her brain SPECT imaging studies, which showed low activity levels in the front part of her brain, especially when she tried to concentrate. In people who don’t have ADD, concentration typically activates an area of the brain called the prefrontal cortex (PFC), which is involved with focus, time management, planning, organization, and critical thinking. In people with ADD, however, concentrating actually reduces activity here, making it difficult to pay attention. This is why simply telling someone with ADD to “try harder” or blaming them for not having enough willpower doesn’t help. Brain imaging shows that the harder they try, the worse it gets. Telling someone with ADD to “try harder” or blaming them for not having enough willpower doesn’t help. Brain imaging shows that the harder they try, the worse it gets. The PFC is also involved with sustaining attention span. It trains your mind to focus on important information while filtering out less significant thoughts and sensations. Attention span is required for short-term memory and learning. The PFC, through its many connections within the brain, keeps you on task and allows you to stay with a project until it is finished. The PFC accomplishes this by sending quieting signals to other parts of the brain. In the face of a need to focus, the PFC decreases the distracting input from other brain areas, inhibiting rivals for our attention. However, when the PFC is underactive, less of a filtering mechanism is available and distractibility becomes common. Problems in the PFC often lead to decreased attention span, distractibility, impaired short-term memory, decreased mental speed, apathy, and decreased verbal expression. Underactivity or damage in the PFC can also lead to a decreased ability to express thoughts and feelings. These are things women may experience when they have Inattentive ADD. But they often chalk it up to being lazy, ditzy, or unmotivated. In too many cases, these are unkind labels they have been given by their parents, teachers, or coaches. A large number of the female patients at Amen Clinics who learn they have ADD say that they spent their whole lives thinking they were stupid. If you have undiagnosed ADD, you may feel this way too.ENHANCING BRAIN FUNCTION IN INATTENTIVE ADD
The brain imaging work at Amen Clinics shows that even if your PFC is underactive and you’ve had undetected ADD for decades, you have the opportunity to optimize your brain function and enhance your life. With the right treatment, you can be more focused, more organized, and more motivated to reach your goals. This has positive implications for every area of your life—career, health and fitness, relationships, and self-esteem. Many women assume that medication is the only treatment option for ADD. And some, like Clery, hate the idea of taking stimulant medication. “When I think of ADD I think of Adderall, and Adderall is like legal speed,” says the influencer who openly talks about being a former addict (she’s been sober now for several years). “I think it’s extremely addictive, and I think it can destroy people’s lives if they have that addictive personality like I do.” Neuropsychiatrist Daniel G. Amen, MD, the founder of Amen Clinics and 12-time bestselling author who evaluated Clery, has a different view. He says medication should never be the first or only thing you do for ADD. However, he adds, “Withholding appropriate stimulation from somebody who has sleepy frontal lobes is like withholding glasses from somebody who can’t see.” Dr. Amen is quick to point out that medication is not the only option for treating Inattentive ADD or other types of the condition. At Amen Clinics, the ADD brain enhancement program includes medications (when necessary) but also focuses on natural alternatives to ADD medication, including diet, exercise, supplements, neurofeedback, behavioral interventions, psychological strategies, and more. The good news is Inattentive ADD in women is usually very responsive to the right treatment. With an accurate diagnosis and the proper treatment program, you can change your brain, stop feeling bad about yourself, and start living the life you want. ADD/ADHD—as well as anxiety, depression, and other mental health conditions—can’t wait. At Amen Clinics, we’re here for you. We offer in-clinic brain scanning and appointments, as well as mental telehealth, clinical evaluations, and therapy for adults, teens, children, and couples. Find out more by speaking to a specialist today at 888-288-9834 or visit our contact page here. Smoke and other types of air pollution contain dangerous toxins that can harm the human brain and raise the risk of mental health disorders. According to 2019 research in Environmental Health Perspectives and Plos Biology, areas that have higher levels of environmental pollution are associated with more cases of anxiety, depression, bipolar disorder, psychosis, and suicidal thoughts and behaviors. Despite the emerging evidence, the effects of environmental toxins on mental health remain virtually ignored in traditional psychiatry. Amen Clinics, however, which has the world’s largest database of functional brain scans related to behavior, has been aware of the association between environmental toxins, brain health, and psychiatric and cognitive problems for decades. The team of neuropsychiatrists at Amen Clinics call this phenomenon Toxic Brain.WHAT IS TOXIC BRAIN?
Toxic Brain occurs when environmental toxins harm the brain and contribute to psychiatric or cognitive issues. Environmental toxins impact nearly every aspect of your body and can damage the brain. Toxic Brain occurs when environmental toxins harm the brain and contribute to psychiatric or cognitive issues. On brain SPECT scans, a “scalloped” appearance and overall decreased cerebral blood flow is a sign of possible toxicity. At Amen Clinics, when this pattern is seen, it prompts our team of neuropsychiatrists and integrative medicine (also called functional medicine) physicians to investigate why. Additional testing and a detailed clinical history help determine the root cause of Toxic Brain.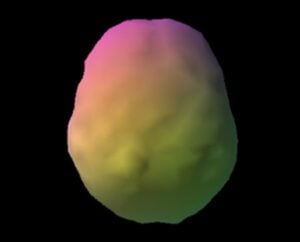
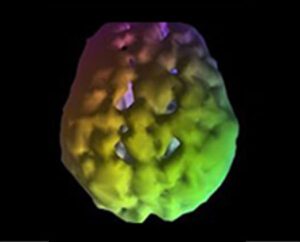 Caption: SPECT (single-photon emission computed tomography) is a nuclear medicine study that evaluates blood flow and activity in the brain. Basically, it shows 3 things: healthy activity, too little activity, or too much activity. The healthy surface brain SPECT scan on the left shows full, even symmetrical activity. The Toxic Brain scan on the right shows scalloping and decreased overall activity and blood flow.
Caption: SPECT (single-photon emission computed tomography) is a nuclear medicine study that evaluates blood flow and activity in the brain. Basically, it shows 3 things: healthy activity, too little activity, or too much activity. The healthy surface brain SPECT scan on the left shows full, even symmetrical activity. The Toxic Brain scan on the right shows scalloping and decreased overall activity and blood flow.
WHAT ARE THE SYMPTOMS OF TOXIC BRAIN?
Exposure to toxins is associated with a variety of physical and psychiatric symptoms. On the physical side, issues can include autoimmune diseases, diabetes, cancer, fatigue, numbness, tingling, tremors, allergies, abdominal pain, diarrhea, smelly stools, bad breath, weight issues, skin rashes, sweats, and more. Research shows that from a psychiatric standpoint, exposure to toxins can increase the risk of:- Anxiety
- Depression
- Suicide
- ADD/ADHD
- Learning problems
- Memory problems and dementia
- Brain fog
- Autism
- Temper outbursts
- Psychotic behavior
HOW TOXIC IS YOUR BRAIN?
Wildfire smoke is only one of many environmental toxins that damage the brain and contribute to mental health problems and cognitive issues. Every single day, we are exposed to a host of chemicals, pesticides, fumes, and products that poison the human brain. Common toxins in the air we breathe, the foods we eat, and the products we rub on our skin are absorbed into our bodies via our lungs, digestive system, and pores and can eventually impact the brain. The more exposure you have to these everyday toxins, the more you’re putting your brain at risk and increasing your chances of mental health issues. Take the following quiz to get a better idea of your brain’s toxic load. The more questions you answer “yes” to, the more toxic your brain is likely to be.- Do you smoke, or are you around secondhand smoke?
- Do you smoke marijuana?
- Do you use conventional cleaning products and inadvertently breathe the fumes?
- Have you been exposed to carbon monoxide?
- Do you travel on planes more than six times a year?
- Do you pump your own gas or breathe automobile exhaust?
- Do you live in an area with moderate to high air pollution or are you being exposed to smoke from wildfires?
- Have you lived or worked in a building that had water damage and mold in it?
- Do you come in contact with flame-resistant clothing or carpet, or with furnishings sprayed with chemicals to prevent stains?
- Do you spray your garden, farm or orchard with pesticides or live near an area with pesticides?
- Do you paint indoors without ventilation?
- Do you have more than four glasses of alcohol a week?
- Do you regularly eat processed or fast foods?
- Do you regularly eat conventionally raised produce, meat, dairy, or farm-raised fish?
- Do you eat large (i.e., mercury-contaminated) fish, such as swordfish?
- Do you eat non-organic fruits and vegetables on a regular basis?
- Do you consume foods with artificial colors or sweeteners, such as diet sodas, or use artificial sweeteners, such as aspartame (NutraSweet), sucralose (Splenda), or saccharin (Sweet’N Low)?
- Do you use more than 2 health and/or beauty products per day? (Most people never read the labels and don’t realize how many chemicals are included)
- Do you live in a house that contains lead pipes or copper plumbing soldered with lead (built prior to 1978)?
- Do you wear lipstick or kiss someone with lipstick made with lead (60% of the lipstick sold in the U.S. contains lead)?
- Do you have mercury amalgam fillings? How many?
- Do you work in a job where you are exposed to environmental toxins, such as firefighting, painting, welding, longshoreman?
- Have you had general anesthesia? How many times?
HOW TO HEAL FROM TOXIC BRAIN
If your brain has been chronically exposed to environmental toxins and you’re experiencing psychiatric or cognitive symptoms, it’s important to investigate further. SPECT imaging can help determine if there is the telltale scalloping pattern and reduced overall activity typically seen in Toxic Brain and can provide valuable insights into other conditions. Even if your brain does look toxic, don’t despair. There is hope. You can heal your brain. Here are some of the recommended interventions:1. Limit or eliminate your exposure to toxins.
You can’t completely avoid toxins—especially during times when massive wildfires are spewing unhealthy toxins into the air you breathe—but you can limit your exposure. Here are some of the best ways to detox your brain, your body, and your life.- Quit smoking, stop using marijuana and limit alcohol to 2-4 glasses a week.
- Remove “silver” dental fillings.
- Reduce your consumption of toxin-contaminated foods.
- Choose organic foods when possible.
- Always wash your fruits and vegetables.
- Avoid processed foods and those with chemical ingredients.
- Choose meat and dairy that is antibiotic and hormone-free.
- Drink 3-4 quarts of clean water a day.
- Check your home for mold and eliminate it.
- Use an air purifier.
- Do a bathroom cleanse to eliminate unsafe cleaning and personal care products (use the Think Dirty app).
2. Start a brain rehab program.
- Fall in love with your brain.
- Avoid things that hurt your brain.
- Adopt habits that help the brain.
- Consider neurofeedback.
- Try hyperbaric oxygen therapy (HBOT), which can speed the healing of the brain.
- Take brain-enhancing supplements, such as omega-3 fatty acids.
What is Bipolar Disorder?
Bipolar disorder is a cyclic mood disorder that includes both manic episodes and depressive episodes. These episodes are associated with dramatic changes in moods, energy levels, and activity. Manic episodes are characterized by:- an abnormally elevated mood
- inflated self-esteem
- grandiose ideas
- racing thoughts
- poor judgment that leads to risk-taking behavior
- a decreased need for sleep
- delusions or hallucinations
- sad or negative moods
- loss of interest in usually pleasurable activities
- feelings of helplessness and hopelessness
- decreased energy
- suicidal thoughts and behavior
5 Reasons Why Bipolar Disorder is So Often Misdiagnosed
1. It often starts with depressive symptoms.
One of the reasons why this condition is so often misdiagnosed is because the first signs are often depression rather than mania, according to a review in the journal Psychiatry. This means many people seek treatment for depression and are often prescribed antidepressants, which aren’t effective for bipolar disorder. As a result, nearly 40% of people with bipolar disorder are initially diagnosed with depressive disorder.2. Co-occurring mental health conditions.
Among people with bipolar disorder, 62% also meet the clinical criteria for ADD/ADHD, according to a study in Clinical Psychology. Anxiety disorders, panic disorders, obsessive compulsive disorder, social phobias, eating disorders, and some personality disorders are also seen with bipolar disorder. In children and adolescents, bipolar disorder may also co-exist with oppositional defiant disorder and other conduct disorders.3. Co-existing substance abuse.
Adding to the difficulty of getting an accurate diagnosis is the common abuse of alcohol or drugs among people with bipolar disorder. Some studies have noted that in people with the condition as many as 69% abuse alcohol and up to 60% abuse drugs. Substance use can cause symptoms that are similar to those seen in bipolar disorder, including emotional highs and lows and major swings in energy levels.4. Hidden brain injuries.
At Amen Clinics, the global leader in brain health, brain SPECT imaging reveals that many people who have been diagnosed with bipolar disorder have signs of undetected traumatic brain injury. Head trauma can cause many of the same symptoms seen in bipolar disorder. Among patients at Amen Clinics, healing the brain can be beneficial in decreasing those symptoms.5. Medication isn’t the only option.
In the traditional medical and psychiatric community, bipolar disorder is generally treated with medication. The psychiatrists and physicians at Amen Clinics are not opposed to medication, but it should never be the only thing you do for your condition. Adopting brain healthy habits—including healthy nutrition, exercise, lifestyle changes, nutritional supplements, and helpful forms of therapy— in addition to medication (when necessary) can be powerfully beneficial components of an effective treatment plan for bipolar disorder. Bipolar disorder—as well as ADD/ADHD, anxiety, and other mental health issues—can’t wait. During these uncertain times, your mental well-being is more important than ever and waiting until life gets back to “normal” is likely to make your symptoms worsen over time. At Amen Clinics, we’re here for you. We offer in-clinic brain scanning and appointments, as well as mental telehealth, remote clinical evaluations, and video therapy for adults, children, and couples. Find out more by speaking to a specialist today at 888-288-9834. If all our specialists are busy helping others, you can also schedule a time to talk. During the pandemic, divorce rates have soared by 34%, according to a recent survey. Newlyweds married less than 5 months have been the hardest hit, with twice as many seeking a divorce compared to 2019. And with the pandemic, job losses, and stay-at-home orders, it took only 3 weeks for marriages to fall apart. How’s your relationship holding up with the stacked stresses we’re all facing these days? Have your marital issues become more glaring? Have you tried marriage counseling but haven’t achieved the changes you were hoping for? There are many experienced therapists and counselors who offer solid strategies to improve relationships. With some couples, however, one or both parties can’t seem to follow their recommendations even though they love their partner and want to save the marriage. What’s the problem? It may be due to brain dysfunction. Therapists and counselors don’t look at the brain, so it’s impossible to know if underlying problems in the brain are contributing to marital discord and preventing one or both parties from following their advice. Amen Clinics partners with thousands of therapists and counselors, performing brain SPECT imaging on couples who aren’t making progress in counseling. The scans often reveal areas of the brain that are either overactive or underactive, contributing to problems. Based on the Amen Clinics database of over 160,000 brain scans, here are the 5 most common brain regions where abnormal activity levels can sabotage a relationship. Here are the 5 most common brain regions where abnormal activity levels can sabotage a relationship: Prefrontal cortex, Anterior cingulate gyrus, Deep limbic system, Basal ganglia, Temporal lobes.The 5 Most Common Brain Regions Where Abnormal Activity Levels Can Sabotage A Relationship
1. Prefrontal Cortex (PFC) Problems in Relationships
Located behind the forehead, involved in impulse control, judgment, forethought When the PFC is underactive, people tend to be impulsive in what they say or do, often causing serious problems in relationships. People with a “sleepy” PFC are the type who blurt out hurtful comments without thinking (“You look like you’ve gained weight.”). In some cases, they may impulsively have extramarital affairs without thinking about the consequences of their actions. They may also have trouble paying attention to their partner. Expressing thoughts and feelings can be difficult, causing their partners to complain about a lack of meaningful conversation in the relationship. Sleepy PFC types may have trouble staying on task and finishing projects, following through on commitments, or completing chores, which irritates partners. Being late is also common as is an unconscious tendency to be conflict seeking or to look for problems when none exists. At Amen Clinics, this is called the “let’s have a problem game,” and it can destroy relationships. What their partners say: “She never pays attention to me.” “He says such mean things, it really hurts my feelings.” Optimize it: The nutritional supplement rhodiola, green tea, a higher protein diet, and physical exercise can boost activity in the PFC. When the PFC is optimized, people are able to think before they say or do things and they learn from their mistakes. And they are less likely to seek out conflict, tension, or turmoil. This makes for a more peaceful relationship.2. Anterior Cingulate Gyrus (ACG) Problems in Relationships
Runs lengthwise through the deep parts of the frontal lobes, acts as the brain’s gear shifter Where there is too much activity in the ACG, people tend to be rigid, inflexible, and unbending—“It’s my way or the highway.” They may have obsessive or compulsive tendencies and when things don’t go their way, they may get very upset. Partners of people with an overactive ACG often describe them as uncooperative, difficult, or argumentative. That can be challenging for any relationship. These people don’t like change or trying new things, so spouses can feel like they’re stuck in the same old routine. They also worry a lot, hold onto grudges, can’t let go of past hurts, and are unforgiving of perceived wrongdoings. This means their partners are constantly being reminded about something they did long ago. What their partners say: “She brings up issues from years and years ago.” “He can never say he’s sorry.” Optimize it: The nutraceuticals 5-HTP and saffron and a diet higher in complex carbohydrates can help calm an overactive ACG. When the ACG is optimized, people tend to be more flexible and adaptable, even with the normal ups and downs of relationships. They’re more able to forgive the mistakes of others and can let go of past hurts.3. Deep Limbic System Problems in Relationships
Located near the center of the brain, involved in setting a person’s emotional tone When the limbic system is overactive, there is a tendency toward depression, negativity, and distance from others. They may have trouble bonding with their partner. These people are experts at noticing what’s wrong, including their partner’s flaws, which is usually not helpful. They aren’t playful, don’t feel sexy, and may shy away from sexual activity due to a lack of interest. Low energy levels and low motivation are common in these people, which can put a damper on a relationship. What their partners say: “He doesn’t want to be around other people.” “She’s so negative, it’s hard to be around her.” Optimize it: Physical exercise, aromatherapy, and natural supplements like saffron, DL-phenylalanine, SAMe, and L-tyrosine can be effective in balancing activity in the limbic system. When the limbic system is optimized, people tend to be more positive and better able to connect to their partner. They’re more likely to have better energy and are more playful and interested in sexual activity. Their positive attitude makes them more attractive to others.4. Basal Ganglia Problems in Relationships
Located toward the center of the brain surrounding the limbic system, involved with integrating feelings, thoughts, and movement When the basal ganglia are overactive, there is a tendency toward anxiety, panic, fear, and tension. People often have decreased sexual interest because their bodies tend to be wrapped in tension, such as backaches, headaches, upset stomach, and other physical complaints. They often don’t have the physical or emotional energy to feel sexy or sexual. Most of their memories are filled with anxiety or fear. They can be conflict-avoidant, which can result in relationship problems building up until they seem insurmountable. They have a tendency to be people-pleasers, so they may take on too much responsibility in a partnership then develop feelings of resentment. And they tend to wear out their partners with the constant fear they project. What their partners say: “He predicts the worst possible outcomes to situations.” “She’s so uptight.” Optimize it: Hypnosis, meditation, relaxation training, and the nutritional supplement GABA can help calm overactivity in the basal ganglia. When this region is optimized, people tend to be calmer, more relaxed, and have a more hopeful outlook. Their bodies tend to feel good, making them freer to express their sexuality. And they’re able to deal with conflict in an effective way and speak up for themselves so there is more equal footing in the relationship.5. Temporal Lobe Problems in Relationships
Located underneath the temples and behind the eyes, involved in mood stability, reading social cues, memory, and language When the temporal lobes aren’t functioning properly, people tend to have memory struggles—forgetting anniversaries, birthdays, and other important things that can make loved ones feel neglected and unloved. They often have emotional ups and downs, and it can be hard for a partner to deal with the mood swings. They tend to be temperamental and have problems with anger and can lash out over seemingly small things. This means significant others often feel like they have to walk on eggshells around them. They may take things the wrong way or misread the emotions of others, which can lead to conflict. What their partners say: “I feel like I’m always waiting for him to lose his temper.” “She’s so moody I never know who I’m going to wake up to.” Optimize it: A higher protein diet, anger management, and music therapy can help balance the temporal lobes. When the temporal lobes are optimized, people tend to be more stable emotionally, which helps foster stability in relationships. They tend to have accurate memories and are able to read emotional cues. And they have better control over their temper, which makes everyone around them less on edge. At Amen Clinics, it has been noted that when relationships are crumbling, it’s often because both individuals have brain health issues. When your partner’s brain health issues conflict with your own trouble spots, it can create big problems. Looking at the brains of both people is often beneficial and sometimes very surprising. Marital conflict and relationship issues, anxiety, depression, ADD/ADHD, and other mental health issues can’t wait. During these uncertain times, your relationships and mental well-being are more important than ever and waiting until life gets back to “normal” is likely to make your situation worse. At Amen Clinics, we’re here for you. We offer in-clinic brain scanning and appointments, as well as mental telehealth, remote clinical evaluations, and video therapy for couples, families, and individuals. Find out more by speaking to a specialist today at 888-288-9834. If all our specialists are busy helping others, you can also schedule a time to talk. by Daniel G. Amen, MD I have a terrible ant infestation in my house, and there’s a terrible ANT infestation in our country that’s driving anxiety, depression, trauma, and grief. ANTs are the automatic negative thoughts that ruin your day, steal your happiness, and prolong grief. These days, ANTs are everywhere. Do any of these thoughts sound familiar? “Nothing will ever be the same.” “Everyone’s going to get COVID and die.” “The economy is ruined. It’ll take years or decades to recover.” “I’ll never get another job.” “I lost my business. I’m a loser. I’m nothing.” “My best friend died of COVID. I’ll never get over it.” “The life I knew is over. I’ll never get used to this new normal.” “There’s so much uncertainty, I can’t handle it.” During the pandemic, mental hygiene is just as important as hand washing. It’s time to disinfect your thoughts and kill the ANTs to overcome anxiety, depression, trauma, and grief. Disinfect your thoughts and kill the ANTs to overcome anxiety, depression, trauma, and grief.WHAT ARE ANTs?
I coined the term ANTs in the early 1990s after a hard day at the office, where I had seen 4 suicidal patients, 2 teens who had run away from home, and 2 couples who hated each other. That evening, when I arrived home and walked into the kitchen, I was greeted by an ant infestation. There were thousands of the pesky invaders, marching in lines on the floor, crawling in the sink, on the countertops, and in the cabinets. As I wetted paper towels and began wiping up the hoard of ants, the acronym ANT came to me—Automatic Negative Thoughts. As I thought about my patients that day, I realized that just like my kitchen, they were also infested with ANTs that were robbing them of their joy and keeping them stuck in hurts from the past.WHY ARE ANTs SO HARMFUL?
Negative thoughts cause your brain to immediately release chemicals that affect every cell in your body, making you feel bad. The opposite is also true—positive, happy, hopeful thoughts release chemicals that make you feel good. Your thought patterns can also have long-term effects. Repetitive negative thinking may promote the buildup of the harmful deposits seen in the brains of people with Alzheimer’s disease and may increase the risk of dementia, according to a 2020 brain imaging study in Alzheimer’s & Dementia.WHY YOU NEED TO ELIMINATE THE ANTs
Just because you have a thought has nothing to do with whether it is true. Thoughts lie. They lie a lot, and it is your uninvestigated or unquestioned thoughts that steal your happiness. If you do not question or correct your erroneous thoughts, you believe them, and you act as if they are 100% true. Allowing yourself to believe every thought you have is the prescription for anxiety disorders, depression, relationship problems, and prolonged grief. You can learn to eliminate the automatic negative thoughts and replace them with more helpful thoughts that give you a more accurate, fair assessment of any situation. This skill alone can completely change your life if you embrace and practice it. Note: I am not a fan of positive thinking. It kills way too many people. I advocate accurate, honest thinking. Some anxiety is absolutely critical to good health and success. Pie-in-the-sky thinking and low levels of anxiety are associated with underestimating risks, a lackadaisical attitude toward your health, and making bad decisions. My ANT killing process is based on the work of two mentors: psychiatrist Aaron Beck, who pioneered a school of psychotherapy called cognitive behavior therapy (CBT), which is an effective treatment for anxiety disorders, depression, relationship problems, and even obesity; and Byron Katie, a teacher, and author.HOW TO KILL THE ANTs
Here are the simple steps to eliminate the ANTs. Whenever you feel sad, mad, nervous, or out of control, do the following:- Write down your automatic negative thoughts (ANTs). The act of writing down the ANTs helps to get the invaders out of your head.
- Identify the ANT species. There are 9 types of ANTs. ANT Types
- All-or-Nothing ANTs: Thinking that things are either all good or all bad
- Less-Than ANTs: Comparing and seeing yourself as less than others
- Just-the-Bad ANTs: Seeing only the bad in a situation
- Guilt-Beating ANTs: Thinking in words like should, must, ought, or have to
- Labeling ANTs: Attaching a negative label to yourself or someone else
- Fortune-Telling ANTs: Predicting the worst possible outcome for a situation with little or no evidence for it
- Mind-Reading ANTs: Believing you know what other people are thinking even though they haven’t told you
- If-Only and I’ll-Be-Happy-When ANTs: Arguing with the past and longing for the future
- Blaming ANTs: Blaming someone else for your problems
- Ask yourself if the thought is true. Are you 100% sure it’s true?
- Ask yourself how you feel when you have the thought. The ask how you would feel without the thought.
- Make ANT-killing a daily habit. Killing the ANTs takes practice. You can’t just do it once and think you’ve mastered your thinking patterns. When you make it a daily practice, you will feel freer, less anxious and depressed, and less trapped in past hurts or losses.
WHAT IMAGING SHOWS ABOUT BRAINS THAT ARE STUCK
Understanding what’s happening in the brain is critical in terms of getting help for your symptoms. Here’s why. People with PTSD are often misdiagnosed with traumatic brain injury (TBI) because the 2 conditions share many overlapping symptoms. Similarly, people with trauma-related depression may be misdiagnosed with ADD/ADHD, bipolar disorder, or even dementia. Getting misdiagnosed means you may be given a treatment plan that isn’t right for your brain. It can stimulate a brain that’s already stuck in overdrive, making you feel even more anxious and on edge. Or, it may further calm a brain that’s already stuck off, making you feel more numb, exhausted, and disoriented. Functional brain SPECT imaging can help. A pair of brain imaging studies from Amen Clinics (published in Plos One and Brain Imaging and Behavior) shows that emotional trauma can leave a lasting imprint on your brain. The study in Plos One found that people with PTSD showed increased in the limbic regions, cingulum, basal ganglia, insula, thalamus, prefrontal cortex, and temporal lobes. And both studies showed that SPECT imaging can distinguish PTSD from TBI with high accuracy. With trauma-related depression, it’s important to differentiate from other mood disorders, such as bipolar disorder, as well as other conditions like ADD/ADHD or dementia. Looking at the brain can help you get a more accurate diagnosis.BALANCE YOUR EMOTIONAL BRAIN
The good news is that if your brain is stuck—either in overdrive or off—you can get it unstuck. And there are many natural ways to help you do it. If your emotional brain seems to be stuck in overdrive, you can calm it with the following:- meditation
- prayer
- hypnosis
- scents, like lavender
- supplements, such as GABA, magnesium, or theanine
- EMDR (a psychotherapeutic technique)
- physical exercise
- upbeat music
- scents, such as peppermint or eucalyptus or
- stimulating supplements, such as rhodiola, green tea, or L-tyrosine
- neurofeedback (a non-invasive, medication-free treatment)
THE MIND MED REVOLUTION
In 1987, with the FDA approval of the blockbuster antidepressant (fluoxetine) Prozac, the mind-drug revolution began to dominate psychiatry. Since the launch of Prozac, antidepressant use in the U.S. has increased by 400% and more than 1 in 10 Americans now takes one. Antidepressants are the second most commonly prescribed drug in the United States, just after cholesterol-lowering drugs, according to a paper in the American Psychological Association. Since the launch of Prozac, antidepressant use in the U.S. has increased 400% and more than 1 in 10 Americans now takes one. After the global success of Prozac, the “chemical imbalance” theory of mental illness burst into the public consciousness, and many people began proactively asking their doctors to fix their low moods with pills. Famously, after actress Carrie Fisher was cremated, her ashes were placed in a green and white Prozac-pill shaped urn. Taking pills may seem like an easier and quicker solution to bad moods than taking the time and effort to develop brain-healthy habits, build skills, or change troublesome behavior. Yet, there is a dark side to the mind-meds that is often overlooked. Thousands of lawsuits claim that Prozac and other psychiatric medications increase violent or suicidal behavior. Virtually all antidepressants and antipsychotic medications have black box warnings, which, in simple terms means the FDA cautions patients in the strongest terms to pay close attention to potentially extremely harmful or dangerous threats to their health. At Amen Clinics, we have published papers on depression (Journal of Alzheimer’s Disease), as well as on ADD/ADHD (Journal of Psychoactive Drugs), revealing the SPECT patterns that are associated with both positive and negative responses to medications.PILL PUSHERS
Despite the problems, the pharmaceutical industry is incredibly successful at marketing psychiatric medications to doctors and the general public. From 1996 to 2005, the industry tripled its marketing budget with a 500% increase in direct-to-consumer advertising. Prescription drug ads often do not adequately explain side effects, and because of repeated exposure, many people tune out those statements at the end of TV commercials, often delivered in a rapid-fire manner, such as, “This drug may cause permanent liver damage, seizures, an allergic reaction that leads to fatal throat swelling and suicidal tendencies.” Patients in the U.S. are more than twice as likely to ask for drugs seen in ads compared with those in Canada, where most direct-to-consumer advertising is prohibited. There is no doubt that psychiatric medication saves lives, especially for people who have more serious mental health disorders (which are really brain health issues), such as bipolar disorder and schizophrenia. Yet, it’s critical to be cautious with antidepressants, because once they are started, they can be hard to stop, and they do not just reset your brain, they change it. A 2017 Oxford University study in the Journal of Affective Disorders found most SSRIs—such as Prozac, Paxil, Zoloft, and Lexapro—do not just decrease negative emotions, they reduce all emotions, including love, happiness, and joy. Participants felt separated from their surroundings and cared less about important things in their daily lives. They felt like their personalities had changed.WHO’S PRESCRIBING ANTIDEPRESSANTS?
One of the most disturbing trends is that nearly 85% of psychiatric medications are prescribed by primary care physicians, nurse practitioners, and physician assistants in short office visits; and 72% of these prescriptions are accompanied by no diagnosis in the charts, according to research in Health Affairs. These medical professionals often do not have the time or specialized training to develop comprehensive treatment plans or to tell you about more natural and safer solutions. Some primary care physicians do a wonderful job handling mental health issues, while others cause more harm than needed.THINK SKILLS, NOT PILLS
As record numbers of people experience depression due to the pandemic, our society does not need more of the same in terms of treatment. When it comes to depression, we need skills, not just pills. When it comes to depression, we need skills, not just pills. It’s time for a new way forward that is rooted in neuroscience and hope. Depression and other psychiatric issues really are so much more than just a “mental illness.” Your brain creates your mind. The issues that affect your mind stem from your brain, your body, your thoughts, your social and work interactions with others, and your deepest sense of meaning and purpose. To fully heal from depression, you need to address all of these factors. Only then can you feel the way you’d like to feel and live the life you desire. Depression, anxiety, and other mental health issues can’t wait. During these uncertain times, your mental well-being is more important than ever and waiting until life gets back to “normal” is likely to make your symptoms worsen over time. At Amen Clinics, we’re here for you. We offer in-clinic brain scanning and appointments, as well as mental telehealth, remote clinical evaluations, and video therapy for adults, children, and couples. Find out more by speaking to a specialist today at 888-288-9834. If all our specialists are busy helping others, you can also schedule a time to talk.By Jennifer Love, MD
You’ve seen the memes: A fully packed stadium with the words: “Alcoholics Anonymous Meeting, 2021.” “If you have a drink in each hand there’s a 100% chance you won’t touch your face!” We’ve updated our vocabulary to include “Quarantini.” Amazon now sells a Sit and Sip Refillable Winebag Chair, which pictures an enormous beanbag the size of a small car, with a woman lounging atop drinking from a plastic tube.
The message is clear: When crisis strikes, drinking is not only socially acceptable but encouraged. A study early on in the pandemic claims 1 in 3 Americans are more likely to drink alcohol during work hours while in lockdown. The numbers vary by states: 38% of California, New York, and Pennsylvania workers are drinking during work; about 50% in Idaho, Kansas, Iowa, and Virginia; and Hawaii “wins” at a reported 67%. The study didn’t even look at non-work hour consumption!
As mental health care providers, we have to take notice.
THE COVID EFFECT ON ALCOHOL AND DRUG USE
You may share my observation that shortly into the COVID crisis many psychiatric patients decompensated and needed increasing amounts of attention and treatment, and many addiction patients seemed to recede into some secret abyss.
I’ve also seen a tide of new patients scheduled by concerned family members because hiding an addiction is a lot more challenging when everyone is stuck in the home together. But COVID fear is also a barrier to treatment, as many families refuse to consider treatment modalities that involve anyone leaving the house, limiting treatment to online support.
I’ve been pushed into a more creative role of trying to invent ways to support the recovery of my patients and encouraging ongoing engagement. I’m certainly stretching my Motivational Interviewing muscles, trying to help people find reasons to change behaviors when many literally have nothing to do. Many of our old standbys of “is your drinking causing any problems with work/social interactions/legally…” may not apply. So how can we comfortably discuss increased alcohol or substance use during the COVID era with patients who aren’t in treatment for any addiction?
Well, substance use is like suicide—asking about it is necessary, and it doesn’t increase the risk of someone trying it. So even if you don’t specialize in treating substance use disorders, with a few tips you can proceed comfortably. Refresh yourself with the basics of helping someone increase their own internal motivation for change.
Here are 5 strategies I use.
5 KEYS FOR TALKING ABOUT SUBSTANCE USE
1. Remember, empathy is key.
I tell my patients from day one that we have a “judgment-free space.” I used to be a chemist, and successful experiments don’t rely on judgment. They rely on observation. I go in with a hypothesis, and it’s either correct or incorrect; there’s no need to be attached to whether I’m right. Either way I’m publishing a paper. If we can cultivate a sense of curiosity about ourselves rather than judgment, motivation for self-exploration increases exponentially. Don’t assume your longtime patients know you won’t judge them. Think about how many of them suffer low self-esteem, negative thoughts, and self-doubt. It needs to be stated.
2. I start by asking questions.
“What do you value? Does your current alcohol consumption fit in with those values?” “If COVID is going to go on for a few years, do you want to spend those years being a daily drinker?” “We’re six months in. Did you ever expect to be a daily or near-daily drinker for that long? I think we’re all thinking about that now—even some of my friends and colleagues!” The purpose is for your patient to discover discrepancies between their values or goals and their behavior.
3. Refrain from argument.
Your patient already knows your opinion on smoking, drinking, using drugs, playing video games, or watching porn 12 hours a day. They aren’t discussing this with you because they don’t know what is best; we, as humans, are just wired not to want to make changes. Confrontation slams the door.
4. Encourage curiosity.
Since we as humans resist change, encourage curiosity about internal resistance. I once did a podcast called “Why don’t I want to do the things I want to do?” I want to eat healthy and exercise, but what I really want is to eat pizza and watch Netflix. Judging the pizza and inactivity doesn’t inspire change, it induces shame, which drives people inward (now curled up on the couch). Being curious about the pizza and inactivity allows someone to explore the thoughts and feelings that contribute to their internal resistance and do what they logically want to do.
5. Support an environment of self-efficacy and optimism.
This is when I bring out my famous (ha!) snorkeling analogy. Yes, the words, “Life is like snorkeling” have escaped my lips more than once, but hear me out. We’re out snorkeling, eyes on the colors—the fish, the coral, watching out for reef sharks—and every once in a while, we have to stop, look up, and see where land is. We have to make sure we haven’t drifted. Sometimes we have to swim over to a new area, and then can start looking down again, getting caught up in the colorful show of life. We will hopefully do this a few times in life—make sure where we are is where we want to be in relation to our “grounding spot.” Are you where you want to be? Are your patients?
About the Author: Jennifer Love, MD, Amen Clinics Orange County, CA
Dr. Jennifer Love is board-certified in psychiatry, addiction psychiatry, and addiction medicine, and is a Diplomate of the American Board of Psychiatry and Neurology and the American Board of Addiction Medicine. Dr. Love is an award-winning researcher and international speaker, interested in the interface between cultural and spiritual factors and overall mental health. She is also suboxone certified. Dr. Love’s work focuses on restoring life balance, brain and body health, and helping her patients improve their functionality and satisfaction in life. She considers a wide range of interventions including nutraceuticals, medication, exercise, yoga, psychotherapy, and sleep/relaxation training. Her specialties include mood disorders, substance use disorders, anxiety disorders, anger and irritability, behavioral addictions, co-occurring pain, and opioid dependence.
Dr. Love is the co-author of When Crisis Strikes: 5 Steps to Heal Your Brain, Body, and Life from Chronic Stress. Stay up to date by following @dr_author_jennifer_love on Instagram.
