

Behavioral Addictions
Behavioral addictions—like compulsive gambling, gaming, or shopping—are complex conditions driven by different brain activity patterns. At Amen Clinics, we go beyond traditional mental health care with advanced brain imaging to identify your unique brain type, allowing us to develop a targeted, effective treatment plan tailored to your needs.
WHAT ARE Behavioral Addictions?
When most people think of addictions, their mind automatically goes to alcohol or drug addiction, but there are other types of addictions too. A behavioral addiction, also known as a process addiction, involves engaging in harmful habits despite the consequences. Stopping the behavior suddenly may result in withdrawal symptoms. You may find the repeated behaviors are temporarily rewarding—a cheap hit of happy—but you may be filled with shame and regret later due to the repercussions of those actions. Like alcohol or drugs, behavioral addictions are mental health conditions. They can worsen any other underlying mental health issues, such as mood disorders, and they ruin lives and devastate families. Just like problems with alcohol abuse, they need to be taken seriously. The mental health professionals at Amen Clinics are here to help.
Who HAS Behavioral Addictions?
Anyone can have a behavioral addiction. Many everyday habits and activities that people engage in on a regular basis can become obsessions or obligations, lead to withdrawal symptoms, and interfere with physical and mental health. Although there are other behavioral addictions, some of the most common ones are listed below. (Please also see further below for more information about these behavioral addictions.)
Most common behavioral addictions:
- Gambling behavior
- Compulsive buying disorder
- Food addiction
- Pornography/sex addiction
- Video game addiction
- Exercise
- Work
- Social media/internet addiction
- Self-harm, such as cutting

CO-EXISTING CONDITIONS
Many people with behavioral addictions also have co-existing conditions, such as:

What are the Core Symptoms?
There are many signs that indicate a favorite activity has gone too far and hijacked the brain’s reward system, including:
- Psychological problems, such as feeling guilty or being unable to stop the behavior.
- Health problems due to the behavior, such as becoming obese from overeating, getting injuries from over-exercising, having sleep problems from too much gaming, or other negative consequences.
- Family dysfunction because of your habit interfering with responsibilities and time that could otherwise be spent with family members and loved ones.
- Personal relationship problems because of affairs or obsession with pornography.
- Financial problems related to shopping addiction or pathological gambling leading to the loss of your home or savings.
- Legal troubles from risky behavior, such as paying for sex with prostitutes or failing to pay debts.

What Causes Behavioral Addictions?
Although there is no single cause for behavioral addictions, experts have identified numerous risk factors. These include a genetic predisposition for addictive behaviors, such as a family history of alcohol abuse or other substance use disorders, changes in the structure and function of the brain, emotional trauma and other underlying mental disorders, and acute stress.

Why Choose Amen Clinics TO TREAT YOUR Behavioral Addictions?
At Amen Clinics, our brain-imaging work has helped us identify 6 types of brain patterns associated with behavioral addictions. When it comes to treatment methods, one size does not fit all! What works for one person with a behavioral addiction may not work for another—or could even make your symptoms worse! Based on your type, we can create a personalized behavioral addiction treatment plan using the least toxic, most effective therapies and strategies to optimize your brain and help you regain control of your life.
ADDICTED BRAINS WORK DIFFERENTLY
Brain dysfunction is the #1 reason why people fall victim to addiction. As with all mental health disorders, your brain plays a central role in your vulnerability to addictive disorders and your ability to recover and avoid harmful behaviors. Behavioral addictions involve multiple areas of the brain, including the prefrontal cortex (PFC), anterior cingulate gyrus (ACG), nucleus accumbens, amygdala, and hippocampus.
SPECT (single photon emission computed tomography) is a nuclear medicine study that evaluates blood flow and activity in the brain. Basically, it shows three things: healthy activity, too little activity, or too much activity. The healthy surface brain SPECT scan on the top right shows full, even, symmetrical activity. The brain scan below it from a person with sex addiction, brain trauma, ADHD, and drug abuse (cocaine) shows lower overall activity, including in the PFC. Low activity in the PFC is associated with impulsive behavior.
Healthy Brain Scan
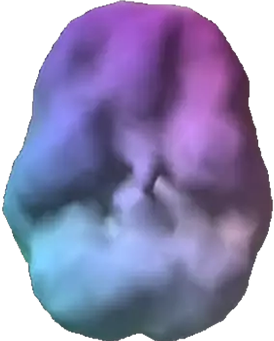
Addicted Brain Scan
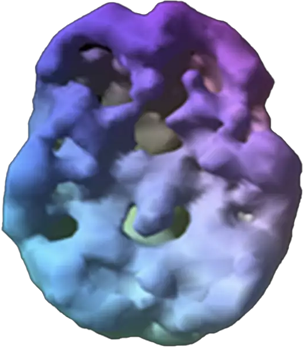
6 Types of Behavioral Addictions
Behavioral addiction is not a single or simple mental health condition. There are multiple types, and each type requires its own targeted treatment plan. Giving everyone with a behavioral addiction the same treatment will never work, and could even lead to negative consequences. You can learn about the 6 types of behavioral addicts in the section below.
Type 1: COMPULSIVE ADDICTS
People with this type have trouble shifting their attention and tend to get stuck on obsessive thoughts of gambling, internet porn, food, or non-substance addictions. Regardless of what they are addicted to, the thinking pattern and basic mechanisms are the same for their compulsive behavior. They tend to get locked into one course of action and have trouble seeing options. The most common brain SPECT finding in this type is increased anterior cingulate gyrus activity, which is most commonly caused by low brain serotonin levels. This finding is similar to what we see with obsessive-compulsive disorder
Type 2: IMPULSIVE ADDICTS
People with this type have trouble with impulse control even though they may start each day with the intention of refraining from their addictive behavior. The most common SPECT finding for this type is low activity in the prefrontal cortex (PFC), likely due to low levels of dopamine.
The PFC acts as the brain’s supervisor and is involved in impulse control, judgment, planning, follow-through, decision-making, and attention. When the PFC is underactive, people can be easily distracted, bored, inattentive, and impulsive. This type is often seen in conjunction with ADHD/ADD and is more common in males.
Type 3: IMPULSIVE-COMPULSIVE ADDICTS
People with this type have a combination of both impulsive and compulsive behavior. The brain SPECT scans tend to show low activity in the prefrontal cortex (associated with impulsivity, likely due to low dopamine levels) and too much activity in the anterior cingulate gyrus (associated with compulsivity and low serotonin levels). This pattern is common in the children and grandchildren of those with alcohol use disorder.
Type 4: SAD OR EMOTIONAL ADDICTS
People with this type often have a behavioral addiction characterized by the use of food to medicate underlying feelings of depression, boredom, or loneliness, leading to a worsening of mental and physical health issues. This type is more commonly seen in women. The typical SPECT findings associated with this type are increased activity in the deep limbic system and low activity in the prefrontal cortex.
Type 5: ANXIOUS ADDICTS
People with this type tend to engage in behaviors or use food to medicate underlying feelings of anxiety, tension, nervousness, and fear. More commonly seen in women, this type tends to suffer physical symptoms of anxiety, such as muscle tension, headaches, stomachaches, and heart palpitations. People with this type tend to predict the worst and may be excessively shy or easily startled. The SPECT finding that correlates to this type is too much activity in the basal ganglia, likely due to low levels of GABA.
Type 6: TEMPORAL LOBE ADDICTS
People with this type tend to have problems with temper, mood swings, learning, and memory. Abnormal activity in the temporal lobes is commonly due to past head injuries, infections, a lack of oxygen, exposure to environmental toxins (such as toxic mold), or it may be inherited. The SPECT findings typically show decreased activity in the temporal lobes, although sometimes increased activity is present.
Common Behavioral Addictions
Many everyday habits and activities that people engage in on a regular basis can become obsessions or obligations, and turn into mental health conditions that require behavior addiction treatment. Some of the most common behavioral addictions include:
Gambling: Approximately 2-3 percent of Americans have a gambling problem.
Food: It’s unclear exactly how many people suffer from food addictions, but over one-third of American adults and 18.5 percent of kids and adolescents are obese.
Sex and Pornography: An estimated 3-6 percent of Americans engage in compulsive sexual behavior, and although there are no definitive statistics on pornography addiction, a growing number of men are seeking help for the condition.
Video Gaming: A 2016 study on 3,389 video gamers found that 1.4 percent of them were addicted to gaming and 7.3 percent were considered problem gamers.
Exercise: Among people who go to the gym, about 3 percent are estimated to be addicted to working out. Among marathon runners and triathletes, the rate of addiction to exercise jumps to 50 percent and 52 percent, respectively.
Work: The U.S. has some of the highest rates in the world of workaholics, or compulsive workers. This behavior prevents them from partaking in other activities (such as being with their family).
Internet/Social Media: It is estimated that about 12 percent of social media users have an addiction to it.
Self-Harm: Approximately two million reports of self-harm are made each year in the U.S. It is more common in women, with about one in five females engaging in the behavior compared with one in seven males.
WANT TO LEARN MORE? DOWNLOAD OUR 6 TYPES OF ADDICTions EBOOK

