

Lyme Disease and Other Infections
Lyme disease and other infections can produce symptoms that closely mimic mental health disorders. As a result, the true underlying cause is often overlooked or misdiagnosed. At Amen Clinics, we use advanced brain-imaging technology to detect patterns that may be associated with infectious processes, leading to a more accurate diagnosis and a more effective treatment plan.
WHAT IS LYME DISEASE?
Lyme disease is a bacterial infection caused by the bite of an infected tick. More specifically, blacklegged ticks (also known as a deer ticks) found throughout the eastern half of the country and Western blacklegged ticks which populate the Pacific coastal areas can be carriers of Borrelia burgdorferi, the bacteria that causes Lyme disease in the U.S. It has been vastly underdiagnosed due to delayed or inadequate testing methods and a general lack of acknowledgement about Lyme disease by the medical community—especially in areas that are less vulnerable to tick-borne illnesses.
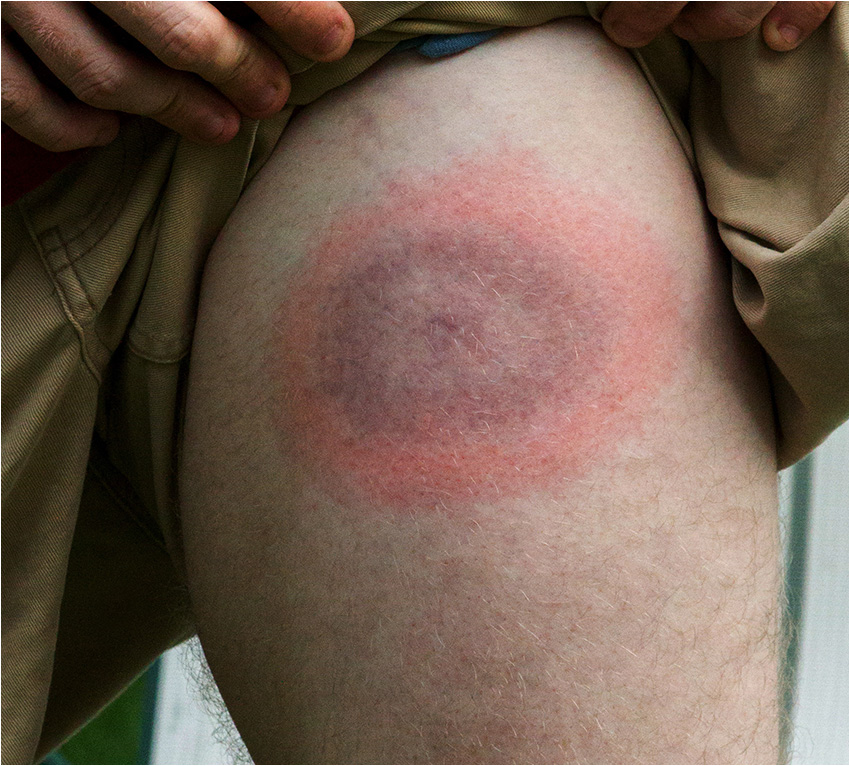
If an infection is caught early, antibiotics can often successfully treat it and diminish the chances of lasting problems. Unfortunately, many people don’t notice when they have been bitten by a tick, and not everyone who is infected with the bacteria will develop the tell-tale bullseye rash. To further complicate things, once a tick bites and is attached to the skin, it won’t cause a Lyme infection for at least 24 hours and symptoms may not emerge for a few days or even a month. Because of this delay, the possibility of Lyme disease can easily be overlooked. Furthermore, the bacteria can become dormant, hiding in cells of the central nervous system, including the brain, for months or years.
Consequently, when it remains undiagnosed, the infection festers, wreaking havoc on the immune system and causing a host of inflammatory responses which can impair healthy brain function. For example, 70% of those affected with Lyme disease report changes in their thinking, such as memory loss and reduced mental sharpness.
Who has Lyme Disease?
People who are active outdoors are more at risk for Lyme disease—especially when preventative measures to protect against tick bites aren’t utilized. Since children spend a lot of time outside, those between the age of 3 and 14 are at the greatest risk followed by people over 50, who enjoy hiking or other outdoor activities such as gardening or playing golf. Those who work outside in grassy areas or other known tick habitats are susceptible too, but anyone can get a tick bite—even in their own yard. There are an estimated 427,000 new cases of Lyme disease each year in the United States.
What are Potential Symptoms of Untreated Lyme Disease and Other Infections?
It is well known that Lyme disease and other infections can cause physiological symptoms, including fever, swollen glands, sore throat, breathing problems, headache, and joint pain or swelling. But many people are unaware that they can also lead to cognitive and neuropsychiatric issues, including:

- Poor judgment
- Memory problems
- Short attention span
- Trouble with focus & concentration
- Poor decision-making
abilities - Slower mental
processing speed - Impaired speech
functions
- Changes in personality
- Hallucinations
- Problems sleeping
- Decreased libido
- Addictive behaviors
- Disorientation
- Violence
- Suicide

Lyme disease can be misdiagnosed or lead to the following if it goes untreated:
- Clinical Depression
- Bipolar Disorder
- Anxiety Disorders
- Posttraumatic Stress Disorder (PTSD)
- Schizophrenia
- Psychosis
- Alzheimer’s Disease
- Developmental Disorders
- Autism Spectrum Disorder
- Eating Disorders

Why Choose Amen Clinics for Treating Lyme Disease and Other Infections?
At Amen Clinics, we have extensive experience diagnosing and treating Lyme disease and other infections, and particularly the neuropsychiatric symptoms these illnesses can cause. Unlike traditional psychiatry, which remains the only medical specialty that rarely looks at the organ it treats, Amen Clinics uses brain SPECT imaging to take the guesswork out of psychiatry. Based on our brain-imaging work—nearly 300,000 functional brain scans and growing—we can identify patterns in the brain that suggest an infection may be the root cause of symptoms.
Infected Brains Work Differently
On brain SPECT scans, infections in the brain can appear as an overall pattern of significantly high or low blood flow. When these abnormal brain patterns are visible, it indicates a potentially infectious process at work. When we see evidence of infectious disease on SPECT scans, we investigate further with additional testing.
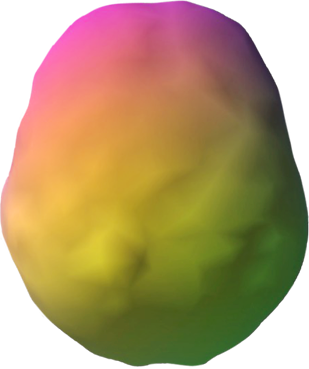
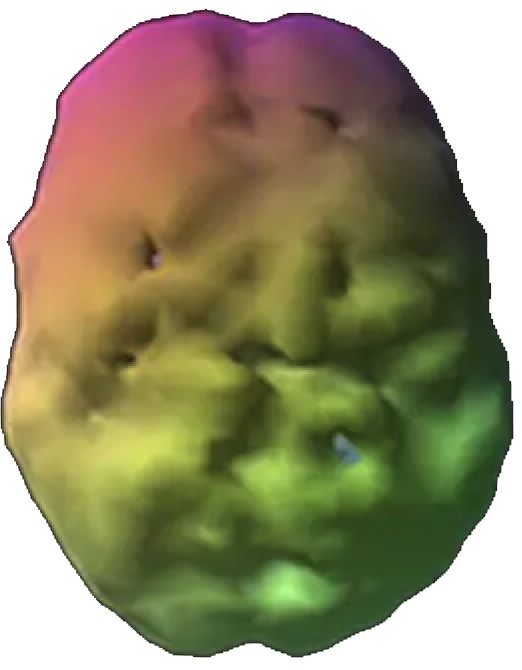
SPECT (single photon emission computed tomography) is a nuclear medicine study that evaluates activity (blood flow) in the brain. Basically, it shows three things: healthy activity, too little activity, or too much activity. The healthy surface brain SPECT scan on the top right looking down from the top, shows full, even symmetrical activity. The scan below it, which is of a patient with Lyme disease, shows overall decreased blood flow denoted by the bumpy appearance on the surface of the brain. The pattern on this scan shows low activity due to the infection.
Healthy Brain Scan
Lyme Disease Brain Scan
Lyme Disease & Other Infectious Agents
Lyme disease isn’t the only infection that can interfere with brain function. Other infectious agents can also cause inflammation and lead to brain disorders, which can mimic or cause a multitude of symptoms associated with mental health conditions. Because of this, people with these infections are often misdiagnosed with psychiatric disorders.
Traditionally, the medical community has dismissed the fact that infections can be associated with these types of symptoms, but that is changing. An editorial in the Journal of Alzheimer’s Disease written by a worldwide group of 33 scientists suggested the medical community has been neglecting to look at infectious diseases as a root cause of many memory problems, including Alzheimer’s disease and other dementias.
Other Infections that can Harm Brain Function
Bacteria, parasites, viruses, and other infectious agents that can cause inflammation and lead to brain disorders, include (but are not limited to):
- Streptococcus—strep throat or scarlet fever
- Toxoplasma gondii—a tiny single-celled parasite that is often carried in cats and shed in their feces
- West Nile virus—a mosquito-borne disease
- Meningitis—inflammation of the tissues surrounding the brain and spinal cord
- Herpes family viruses, such as Epstein-Barr, cytomegalovirus, herpes simplex virus-1 (most often as cold sores), and herpes simplex virus-2 (genital or buttock lesions)
- HIV/AIDS
- COVID-19 and long COVID
- Syphilis
- Other tick-borne illnesses, including Rocky Mountain spotted fever, anaplasmosis, ehrlichiosis, and Powassan virus
- Helicobacter pylori (common cause of peptic ulcers)
- Chlamydophila pneumoniae (type of bacteria that causes pneumonia)
- Influenza—the common flu bug
Neuropsychiatric Symptoms of Streptococcus and Toxoplasma Gondii
Like Lyme disease, other infections can cause neuropsychiatric symptoms. For example,
Streptococcus bacterial infection that leads to PANDAS (pediatric autoimmune neuropsychiatric disorders associated with streptococcal infections) can cause a sudden onset of symptoms, such as:
- Obsessive thoughts
- Compulsive rituals
- Overwhelming fears
- Moodiness or irritability
- Motor or vocal tics
- Hyperactive behavior
- Motor skill problems
Streptococcus infection can be misdiagnosed as or lead to:
- Brain fog
- Fatigue
- Concentration issues
- Memory problems
Toxoplasma gondii can cause cysts to develop in the brain and other organs, leading to a condition called toxoplasmosis. Symptoms of toxoplasmosis include:
- Impulsive behavior
- Dramatic mood swings
- Hallucinations
- Memory problems
- Anxiety
- Obsessive thoughts
- Compulsive rituals
- Suicidal thoughts
Toxoplasma gondii can be misdiagnosed as or lead to:
- Schizophrenia
- Bipolar disorder
- Anxiety disorders
- Depression
- Alzheimer’s disease
- Parkinson’s disease
The Consequences of Improper Diagnosis and Treatment
When people with undetected Lyme disease or other infections are misdiagnosed with mental health disorders or cognitive dysfunction, treatments often don’t work. And in some cases, they can make symptoms worse. Without a correct diagnosis and the appropriate treatment, the infection persists, causing further injury to the brain.
This can eventually lead to trouble in all areas of your life, including decreased productivity at work, poor school performance, and problems with personal and interpersonal functioning. Without getting the right treatment, Lyme disease and other infections can steal your mind and steal your life.
For people who are not responding to treatment for their symptoms, it is very important to investigate whether an underlying infection may be contributing to the issue.


