
Going through emotional trauma or grief can leave a lasting imprint on the brain. In order to properly heal it, it is critical to get the right diagnosis. It is critically important because the symptoms of PTSD and traumatic brain injury (TBI) often overlap (anxiety, depression, irritability, headaches, and insomnia), but the treatments are very different. In fact, treating PTSD as if it is a TBI, or vice versa, can actually make people worse, which is why we believe neuro- imaging studies are so important when people struggle and find that the simple treatments to feel better fast are ineffective.
As mentioned in Dr. Daniel Amen’s new book, “Feel Better Fast and Make it Last,” overcoming trauma and grief is often mislabeled as depression, ADHD, PTSD, panic disorder, and other psychiatric conditions. If you experience symptoms of these conditions after a loss, consider doing grief work before taking medication. If grief is misdiagnosed, psychotropic medications can get in the way of or even prolong recovery.
Meet Steven
On July 16, 2003, Steven, a 33-year-old bicycle repair mechanic working in Santa Monica, California, insisted on having an early lunch. He was not sure why, but he felt drawn to the Santa Monica Farmers’ Market, so he headed there on foot. As he arrived, George Russell Weller, 86, lost control of his car and barreled through the three-block-long farmers’ market. Steven later said, “I thought he was going to run over my legs, I thought I would lose my legs.” At the last possible moment, he managed to jump out of the way. In the chaos, 10 people were killed, and more than 50 were injured. Steven, who had been a military tank commander in the first Gulf War, used the medical skills he had learned to help save others. Still, a woman died in his arms.
Traumatized, Steven went back to work that same day. But for months afterward he couldn’t sleep and couldn’t stop his hands from shaking. By chance, Linda Alvarez, a Los Angeles CBS News anchor, took her bicycle to Steven’s shop shortly after the disaster and discussed it with him in a brief conversation. As they talked, Linda noticed that Steven was shaking. “It started that day,” Steven said.
The image of Steven’s hands stayed with Linda as she believed he may need help overcoming trauma. A month later, while working on another story, Linda learned about work Amen Clinics was doing with a treatment technique called Eye Movement Desensitization and Reprocessing, or EMDR, planting the seed for a story about the treatment and Steven’s trauma.
EDMR: A Powerful Tool To Feel Better Fast and Make It Last
EMDR is an effective psychological treatment developed by Francine Shapiro, a psychologist. In 1987, during a walk around a lake, she noticed that a disturbing thought disappeared when her eyes spontaneously started to move back and forth from the lower left to the upper right visual fields. She tried the eye movements again with another anxiety-provoking thought and found that the anxious feeling went away. In the days that followed, Francine tried the technique with friends, acquaintances, and interested students and found that it was helpful in relieving anxiety. She went on to work with patients and developed a technique that is now used worldwide.
This form of therapy is based on research suggesting that traumatic events can prevent the brain from processing information as it normally does, which results in these events getting “stuck” in the brain’s information processing center. Then, when someone who experienced a trauma recalls it, the memory triggers an intense re-experiencing of the original event, complete with all of its upsetting sights, sounds, smells, thoughts, and feelings.
What Happens During an EMDR Session?
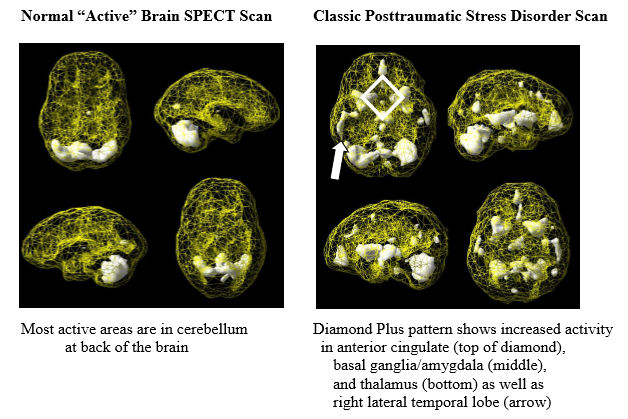
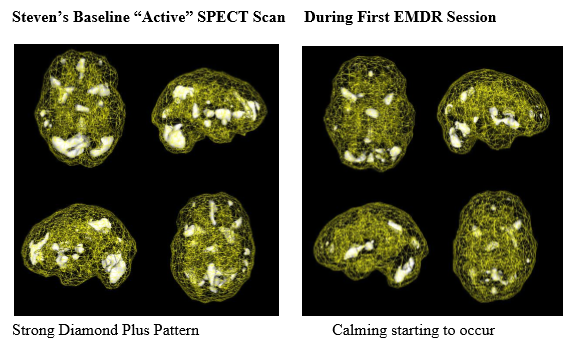
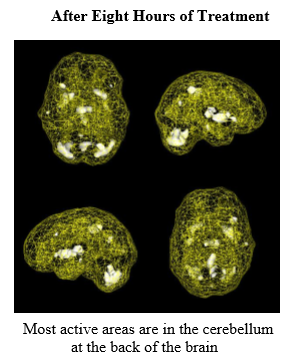
As part of his evaluation, we scanned Steven three times: before treatment, during his first EMDR session, and after eight hours of treatments. Initially, Steven’s brain showed the classic PTSD pattern, with his limbic or emotional brain being extremely hyperactive. Using EMDR with him, we cleared out the traumas one by one. His brain showed benefit during the first treatment and was markedly improved after eight hours of treatment.
When we helped Steven calm and balance his brain, he was happier and able to sleep better.
Dealing with a condition like Steven’s can be challenging, especially when symptoms are compounded by other mental health issues. For more information on how SPECT imaging can help provide a customized treatment plan to help heal your brain, call us today at 888-288-9834 or visit us online to schedule a visit.





To help a child recover from trauma, it s important to communicate openly. Let them know that it s normal to feel scared or upset. Your child may also look to you for cues on how they should respond to trauma so let them see you dealing with symptoms in a positive way.
Comment by Maxim — October 29, 2018 @ 2:40 PM
Visualize the energy your trauma took up inside you leaving your body, or perform a ritual of physical release, like (safely) burning a letter you’ve written to the person who hurt you, or casting off the trauma in the form of an object into the sea. You can borrow a ritual from Judaism called Tashlikh. During the period of repentance, many Jews cast off their sins into a natural, flowing body of water in the form of breadcrumbs. Instead of sins, you can cast off traumas and the emotions and sensations that go with them.
Comment by KatalinLennard — November 6, 2018 @ 10:48 PM
My personal journey to health came from receiving Somatic Trauma Resolution therapy where we established connection with my body, relative safety in the moment, then let my body show how it needed to act to move the energy trapped from the trauma. Once I felt more empowered the memories no longer held an emotional or physical charge.
Comment by Char — November 7, 2018 @ 6:00 PM
This was excellent information! All of us need to understand how traumatic events also store in our bodies, and that they can be released. As a therapist working with couples, I also noticed trauma (when triggered) can sabotage relationships. EMDR, Somatic Experiencing, and Brainspotting all help people become aware of how their nervous systems work, and how they can move past trauma. Thank you for this very helpful article!
Comment by Helene Goble — November 14, 2018 @ 12:59 PM
Good job ….keep it up …and thank you so much for nice articles….
Comment by Rupa Amgain — November 18, 2018 @ 4:40 AM
Fantastic information
Comment by Steve Pohlit — December 23, 2018 @ 5:44 PM
Informative article, thank you. I would like to make a point that I haven’t often seen made re EMDR, that it should be used mindfully and with care. I tried it and felt much worse, experiencing physical symptoms that lasted some months. A therapist said that the therapy can be too aggressive for some, in that the treatment itself can re-traumatize. Prior to trying the treatment I viewed it as a possible magic bullet; for me it was not. This could possibly be avoided if therapist and patient both are cautious and attentive to worsening of symptoms.
Comment by Elspeth — February 14, 2019 @ 2:48 AM
We need more mental health discussions on social media our society is in crisis and we are doing nothing please share
Comment by Anne Joy — April 27, 2019 @ 9:52 AM